Visceral Hypersensitivity: When Your Gut Pain Is Real But Your Tests Are Normal

- Published on: 4/April/2026
- Posted By: Arka Health
Introduction
Chronic abdominal pain with normal test results is one of the most frustrating clinical scenarios for both patients and doctors. Many individuals go through multiple investigations such as endoscopy, scans, and blood tests, only to be told that everything looks normal.
Despite this, the pain continues. It is real, persistent, and often debilitating.
This disconnect between symptoms and test results is not a mystery condition. It is increasingly understood as visceral hypersensitivity, a well defined physiological state where the gut becomes overly sensitive to normal internal processes.
Instead of structural damage, the problem lies in how the nervous system processes signals from the gut. This shifts the focus from visible disease to functional dysregulation.
What Is Visceral Hypersensitivity
Visceral hypersensitivity refers to an abnormal increase in pain perception originating from internal organs, particularly the gastrointestinal tract.
In a healthy system, digestion happens quietly in the background. Movement of food, gas, and fluids does not produce pain. In this condition, the same processes trigger exaggerated discomfort.
Two key sensory changes define this state:
Allodynia
Pain from stimuli that should not cause pain, such as gas movement or mild distension.
Hyperalgesia
An exaggerated response to normally painful stimuli, where minor discomfort feels severe.
These changes occur due to sensitisation of the gut nerves and altered processing in the brain.
Functional Disorders vs Structural Disease
To understand this condition clearly, it is important to differentiate between two categories of gastrointestinal disorders.
Structural Disorders
These include ulcers, inflammatory bowel disease, or tumors where visible damage is present.
Functional Disorders
These are now called disorders of gut brain interaction. There is no visible damage, but communication between the gut and brain is altered.
Visceral hypersensitivity is a central feature of these functional disorders, especially in conditions like IBS and functional dyspepsia.
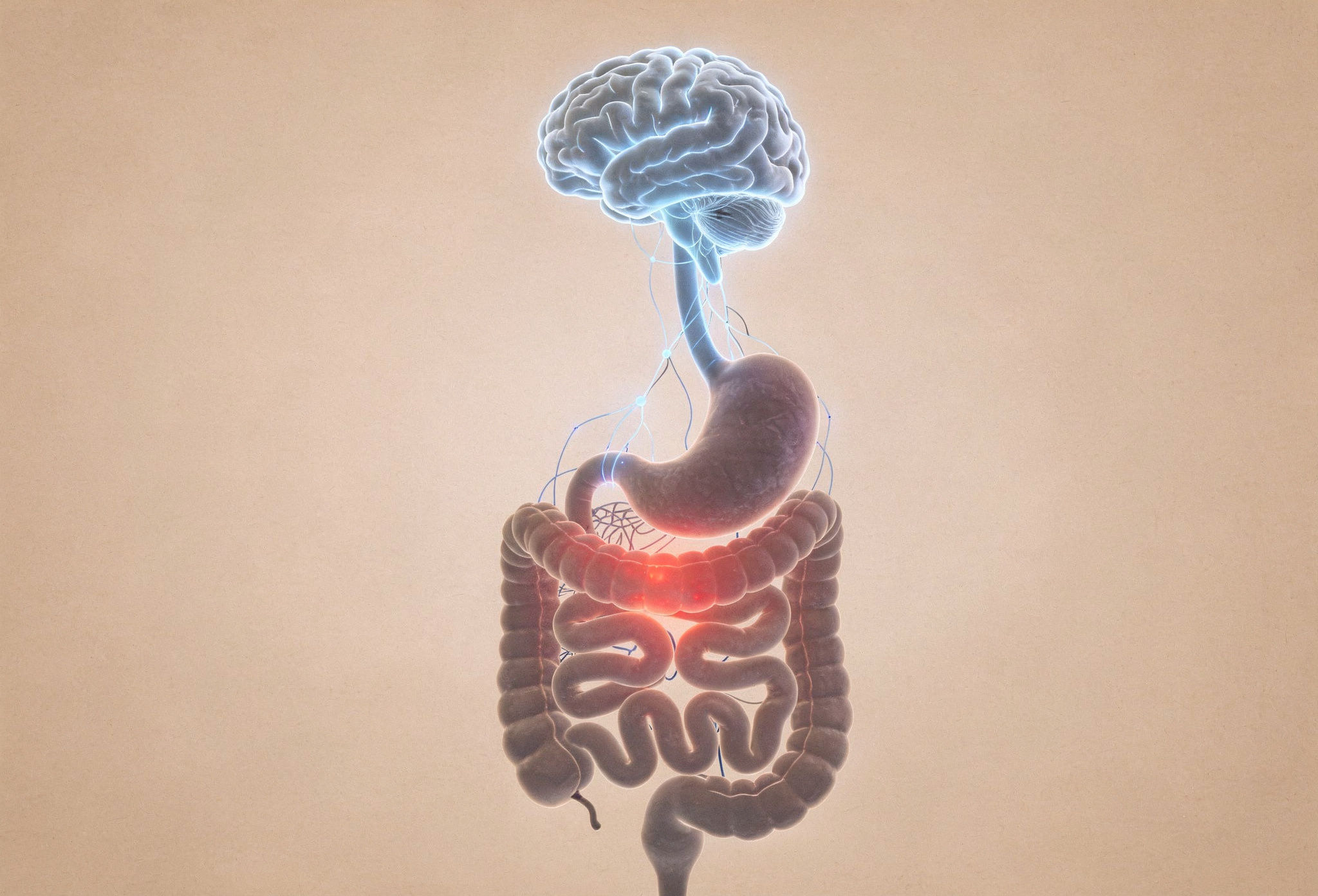
The Gut Brain Axis and Pain Perception

The gut and brain are constantly communicating through neural and hormonal pathways.
In visceral hypersensitivity, this communication becomes distorted.
Signals from the gut are amplified as they travel through:
- Peripheral nerves in the gut wall
- Spinal cord pathways
- Brain regions that interpret pain
This creates a scenario where normal digestive activity is interpreted as pain.
Central Sensitisation: Amplification in the Brain
The second level occurs in the central nervous system.
Repeated signals from the gut cause changes in the spinal cord and brain.
Key Changes Include
- Increased responsiveness of spinal neurons
- Reduced ability of the brain to suppress pain signals
- Heightened activity in emotional processing centers
This means the pain is not only stronger but also more distressing.
How the Condition Develops
Visceral hypersensitivity often begins after a triggering event.
Post Infectious Changes
A common trigger is acute gastroenteritis.
Even after the infection resolves, inflammation and nerve sensitisation can persist. This leads to post-infectious IBS.
Chronic Stress and HPA Axis
Stress plays a major role in maintaining and worsening the condition.
Activation of the HPA axis leads to increased cortisol levels, which affect gut permeability and nerve sensitivity.
Microbiome Imbalance
Changes in gut bacteria influence nerve signaling and immune activation.
An unhealthy microbiome can sustain inflammation and hypersensitivity.
Symptoms and Clinical Presentation
The symptoms are often complex and vary between individuals.
Abdominal Pain Characteristics
- Diffuse and difficult to localise
- Triggered by eating or gas movement
- Fluctuates with stress levels
Digestive Symptoms
- Bloating
- Altered bowel habits
- Urgency
Systemic Features
Because of autonomic involvement, patients may experience:
- Sweating
- Palpitations
- Fatigue
- Sleep disturbances
Overlap Conditions
Visceral hypersensitivity is commonly seen in:
- IBS
- Functional dyspepsia
- Chronic pelvic pain
Why Tests Come Back Normal
Most diagnostic tools are designed to detect structural abnormalities.
They cannot measure nerve sensitivity or gut brain signaling.
This leads to a common clinical gap where:
- Tests appear normal
- Symptoms remain severe
This does not mean the pain is psychological. It reflects a limitation of current diagnostic methods.
Common Mismanagement Issues
Symptom Dismissal
Patients are often told nothing is wrong, which increases anxiety and worsens symptoms.
Repeated Testing
Multiple unnecessary investigations can reinforce fear and delay proper treatment.
Inappropriate Medications
Use of strong painkillers can worsen gut function and sensitivity over time.
Diagnosis Approach
Diagnosis is primarily clinical.
It involves:
- Detailed symptom history
- Identification of pain patterns
- Exclusion of structural disease
A positive diagnosis is based on recognizing features of hypersensitivity, not just ruling out other conditions.
Treatment Strategy
Management requires a multi level approach.
Neuromodulators
Low dose medications help regulate pain signaling.
They reduce nerve excitability rather than treating mood disorders.
Gut Directed Psychological Therapy
Techniques such as cognitive behavioral therapy and hypnotherapy help retrain brain responses.
Dietary Interventions
Low FODMAP diet reduces triggers that cause gas and distension.
Microbiome Support
Probiotics and targeted nutrition help restore gut balance.
Nervous System Regulation
Breathing exercises, biofeedback, and relaxation techniques reduce autonomic overactivity.
Long Term Outlook
Visceral hypersensitivity is a chronic condition, but it is manageable.
With proper treatment, the nervous system can be retrained.
Patients often experience:
- Reduced pain intensity
- Improved digestion
- Better quality of life
ARKA Anugraha Hospital Approach
At ARKA Anugraha Hospital, visceral hypersensitivity is treated as a gut brain axis disorder rather than an unexplained symptom.
The focus is on identifying triggers, understanding nervous system involvement, and addressing both peripheral and central mechanisms.
Dr Gaurang Ramesh and the team use a structured, integrative model that combines clinical gastroenterology with neuromodulation, microbiome therapy, and behavioral interventions.
This approach ensures that treatment is personalized and rooted in both science and patient experience.
Conclusion
Visceral hypersensitivity explains why patients can experience severe gut pain even when all tests appear normal.
It represents a shift from structural diagnosis to functional understanding.
Recognizing this condition allows for targeted, effective treatment that addresses the true source of the problem rather than just managing symptoms.
With the right approach, patients can regain control over their gut health and daily life.
FAQs
1. What is visceral hypersensitivity
It is a condition where the gut becomes overly sensitive to normal digestive processes.
2. Why do tests come back normal
Because standard tests cannot detect nerve sensitivity or gut brain dysfunction.
3. Is the pain psychological
No. It is a biological condition involving nerve sensitisation.
4. What triggers visceral hypersensitivity
Common triggers include infections, stress, and microbiome imbalance.
5. Can stress worsen symptoms
Yes. Stress amplifies gut brain signaling and increases pain perception.
6. How is it diagnosed
Based on symptoms, history, and exclusion of structural disease.
7. What is central sensitisation
It increases pain amplification in the brain and spinal cord.
8. Can diet help
Yes. Dietary changes reduce triggers that activate gut nerves.
9. Are medications required
In many cases, low dose neuromodulators are helpful.
10. Is this condition permanent
Not necessarily. The nervous system can be retrained with proper treatment.
11. Can probiotics help
They support microbiome balance and may reduce symptoms.
12. Is it linked to IBS
Yes. It is a key mechanism in IBS.
13. What is the role of the gut brain axis
It regulates communication between the gut and brain, which is altered in this condition.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
