Is Your IBS Actually an Autoimmune Reaction? The Link Between Gut Inflammation and Immune Dysregulation

- Published on: 03/March/2026
- Posted By: Arka Health

Irritable Bowel Syndrome has long been classified as a functional gastrointestinal disorder, defined primarily by symptoms rather than structural abnormalities. However, emerging evidence is challenging this definition and pushing clinicians to reconsider whether a subset of IBS patients may actually be experiencing an early or low-grade autoimmune response within the gut.
The growing discussion around the IBS autoimmune connection is reshaping how chronic digestive disorders are understood. Instead of viewing IBS as a purely gut-brain axis issue, modern gastroenterology and functional medicine are recognizing the central role of immune activation, intestinal permeability, and microbiome imbalance.
In India, particularly in urban environments, rising exposure to processed diets, stress, and environmental toxins has made this gut-immune interaction even more clinically relevant.
This article explores whether IBS can be linked to autoimmunity, the mechanisms behind this connection, and how a root-cause approach can lead to long-term recovery.
Understanding the IBS–Autoimmune Spectrum
Traditionally, gastrointestinal disorders are divided into two categories:
Functional disorders such as IBS, where no visible structural damage is detected
Organic diseases such as Crohn’s disease or ulcerative colitis, where inflammation and tissue damage are evident
However, this binary classification is increasingly seen as incomplete.
Research shows that many patients diagnosed with IBS exhibit:
Increased mast cell activity in the gut lining
Elevated pro-inflammatory cytokines
Altered immune signaling at the mucosal level
These changes may not be visible on standard diagnostic tests but are sufficient to disrupt gut function and trigger hypersensitivity.
This places IBS on a spectrum where, in some individuals, it may represent a low-grade autoimmune gut disorder rather than a purely functional condition .
The Role of Intestinal Permeability in Autoimmune Activation
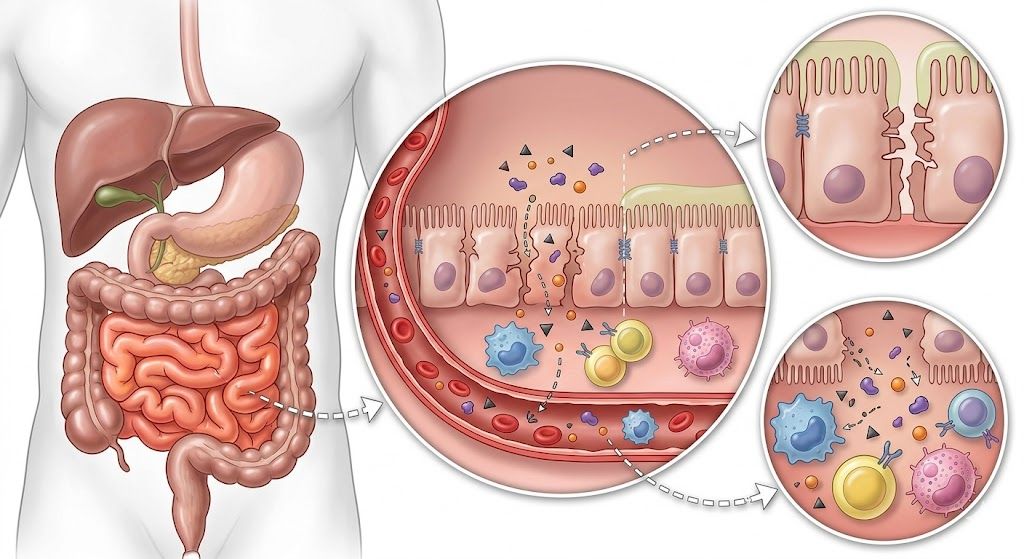
The intestinal barrier is one of the body’s most critical defense systems. It allows nutrient absorption while preventing harmful substances from entering the bloodstream.
This barrier is maintained by tight junction proteins such as zonulin and occludin. When these junctions are disrupted, intestinal permeability increases.
This condition, often referred to as leaky gut, allows:
- Undigested food particles
- Bacterial endotoxins such as lipopolysaccharides
- Environmental toxins
to enter systemic circulation.
The immune system responds aggressively to these intruders. Over time, this chronic immune activation can lead to loss of immune tolerance and the development of autoimmune reactions.
This is a key mechanism behind the leaky gut autoimmune disease model and a central explanation for the IBS autoimmune connection .
Molecular Mimicry and Post-Infectious IBS
One of the most compelling explanations for autoimmune-like IBS is molecular mimicry.
After a gastrointestinal infection, the immune system produces antibodies against bacterial antigens. In some cases, these antigens resemble proteins within the human body.
For example:
- Antibodies targeting bacterial toxins may cross-react with proteins involved in gut motility
- This can disrupt the enteric nervous system
- Resulting in chronic symptoms such as bloating, altered bowel habits, and abdominal pain
This phenomenon explains why many patients report IBS symptoms beginning after food poisoning or infection.
This subtype is often referred to as post-infectious IBS and may represent a form of immune-mediated dysfunction rather than a purely functional disorder.
Gut Dysbiosis and Immune Imbalance
The gut microbiome plays a critical role in regulating immune responses.
In a healthy state:
- Beneficial bacteria produce short-chain fatty acids
- These support regulatory T cells that suppress inflammation
In dysbiosis:
- Harmful bacteria dominate
- Regulatory T cell activity decreases
- Pro-inflammatory Th17 cells increase
This shift leads to systemic inflammation and increases the risk of autoimmune conditions.
Low microbial diversity has been associated with conditions such as:
- Rheumatoid arthritis
- Systemic lupus erythematosus
- Inflammatory bowel disease
This highlights how a localized gut imbalance can have systemic immune consequences .
Progression: From Trigger to Chronic Immune Dysregulation
The transition from normal gut function to immune-driven disease typically follows a pattern:
Acute Phase
- Trigger event such as infection, antibiotics, or stress
- Temporary disruption of microbiome
- Increased intestinal permeability
Chronic Phase
- Persistent dysbiosis
- Ongoing immune activation
- Development of autoantibodies
- Systemic symptoms beyond the gut
Without intervention, this cycle becomes self-perpetuating.
Environmental and Lifestyle Triggers in India
In India, several factors contribute to the rise of autoimmune gut disorders:
- Urban pollution damaging the gut lining
- High intake of processed and refined foods
- Reduced consumption of traditional fermented foods
- Chronic psychological stress
These factors collectively increase intestinal permeability and immune activation, making the IBS autoimmune connection more clinically relevant in metropolitan populations .
Clinical Symptoms: Beyond Digestive Distress
Gastrointestinal Symptoms
- Abdominal pain related to bowel movements
- Chronic bloating and distension
- Diarrhea, constipation, or mixed patterns
- Presence of mucus in stool
Systemic Symptoms
- Chronic fatigue and brain fog
- Joint and muscle pain
- Skin conditions such as eczema or psoriasis
- Nutrient deficiencies including iron and vitamin B12
- Anxiety and mood disturbances
The presence of systemic symptoms often indicates that immune dysregulation is involved, rather than isolated gut dysfunction.
The Gut–Thyroid Axis: A Critical Link

One of the strongest clinical associations is between IBS-like symptoms and thyroid autoimmunity, particularly Hashimoto’s thyroiditis.
Key interactions include:
- Hypothyroidism slows gut motility, leading to constipation and bloating
- Increased intestinal permeability promotes thyroid antibody production
- Dysbiosis contributes to both gut and thyroid dysfunction
This bidirectional relationship creates a cycle where gut and thyroid health continuously influence each other.
Why IBS Is Often Misdiagnosed or Mismanaged
Standard IBS diagnosis relies heavily on symptom-based criteria such as Rome IV guidelines.
Limitations include:
- Lack of evaluation for immune activation
- No assessment of intestinal permeability
- Absence of microbiome analysis
- Over-reliance on symptom suppression
As a result:
- Patients are often told their tests are normal
- Root causes remain unaddressed
- Symptoms persist for years
This highlights the need for a more comprehensive, systems-based approach.
Integrative and Root-Cause Care at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, the approach to IBS and autoimmune gut disorders goes beyond symptom management.
The focus is on identifying and correcting the underlying drivers of disease.
Key components include:
- Advanced diagnostics for gut permeability and microbiome health
- Personalized nutrition strategies to reduce inflammation
- Gut healing protocols to restore barrier integrity
- Immune modulation through targeted therapies
- Mind-body interventions to regulate the gut-brain axis
Specialized programs such as structured gut healing protocols, IV nutrient therapy, and supportive integrative treatments are designed to restore both digestive and immune balance.
Clinical Recommendations for Recovery

For patients suspected of having an IBS autoimmune connection:
- Rule out conditions such as celiac disease and IBD
- Assess intestinal permeability markers
- Restore microbial diversity
- Reduce exposure to dietary and environmental triggers
- Correct micronutrient deficiencies
- Address stress and nervous system imbalance
Recovery requires a multi-dimensional approach rather than a single intervention.
Frequently Asked Questions (FAQ)
- Is IBS an autoimmune disease?
IBS is not officially classified as autoimmune, but many patients show immune activation that mimics autoimmune responses. - What is the IBS autoimmune connection?
It refers to the link between gut inflammation, immune dysregulation, and IBS symptoms. - What causes a leaky gut?
Stress, infections, processed foods, toxins, and antibiotics can increase intestinal permeability. - Can IBS turn into an autoimmune disease?
In some individuals, chronic immune activation may contribute to the development of autoimmune conditions. - What are signs of immune-related IBS?
Symptoms beyond digestion such as fatigue, joint pain, and skin issues suggest immune involvement. - Can gut health affect thyroid function?
Yes, gut dysfunction can trigger thyroid autoimmunity and worsen hypothyroidism. - Is post-infectious IBS autoimmune?
It may involve immune mechanisms such as molecular mimicry. - Can probiotics help autoimmune IBS?
They may help restore microbial balance but should be personalized. - How long does gut healing take?
Initial improvements may occur in 4 to 12 weeks, but full recovery may take longer. - Does stress worsen IBS?
Yes, stress increases gut permeability and inflammation. - Can diet alone fix IBS?
Diet helps but often needs to be combined with immune and gut repair strategies. - What tests identify autoimmune gut issues?
Zonulin, microbiome analysis, and inflammatory markers can provide insights. - Is IBS more common in urban India?
Yes, due to lifestyle, diet, and environmental exposure. - Can autoimmune IBS be reversed?
In many cases, symptoms can be significantly improved with a root-cause approach. - Why are standard tests normal in IBS?
They do not detect microscopic inflammation or immune activity.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
