ECP Therapy for Angina: A Non-Surgical Approach to Managing Chest Pain

- Published on: 17/Feb/2026
- Posted By: Arka Health
Executive Overview
Angina is a manifestation of myocardial ischemia caused by an imbalance between oxygen supply and demand within the heart muscle. While conventional cardiology often focuses on mechanical correction through angioplasty or bypass surgery, growing evidence demonstrates that stable angina is fundamentally a systemic vascular disorder rather than simply a blocked artery problem.
ECP Therapy for angina represents a paradigm shift in cardiovascular care. It offers a non-surgical, physiologically restorative option that improves coronary perfusion, enhances endothelial function, and stimulates natural collateral circulation without invasive intervention.
At ARKA Anugraha Hospital, this therapy is integrated within a broader framework of functional cardiology that addresses inflammation, metabolic dysfunction, and the gut-heart axis to provide sustained cardiac rehabilitation.
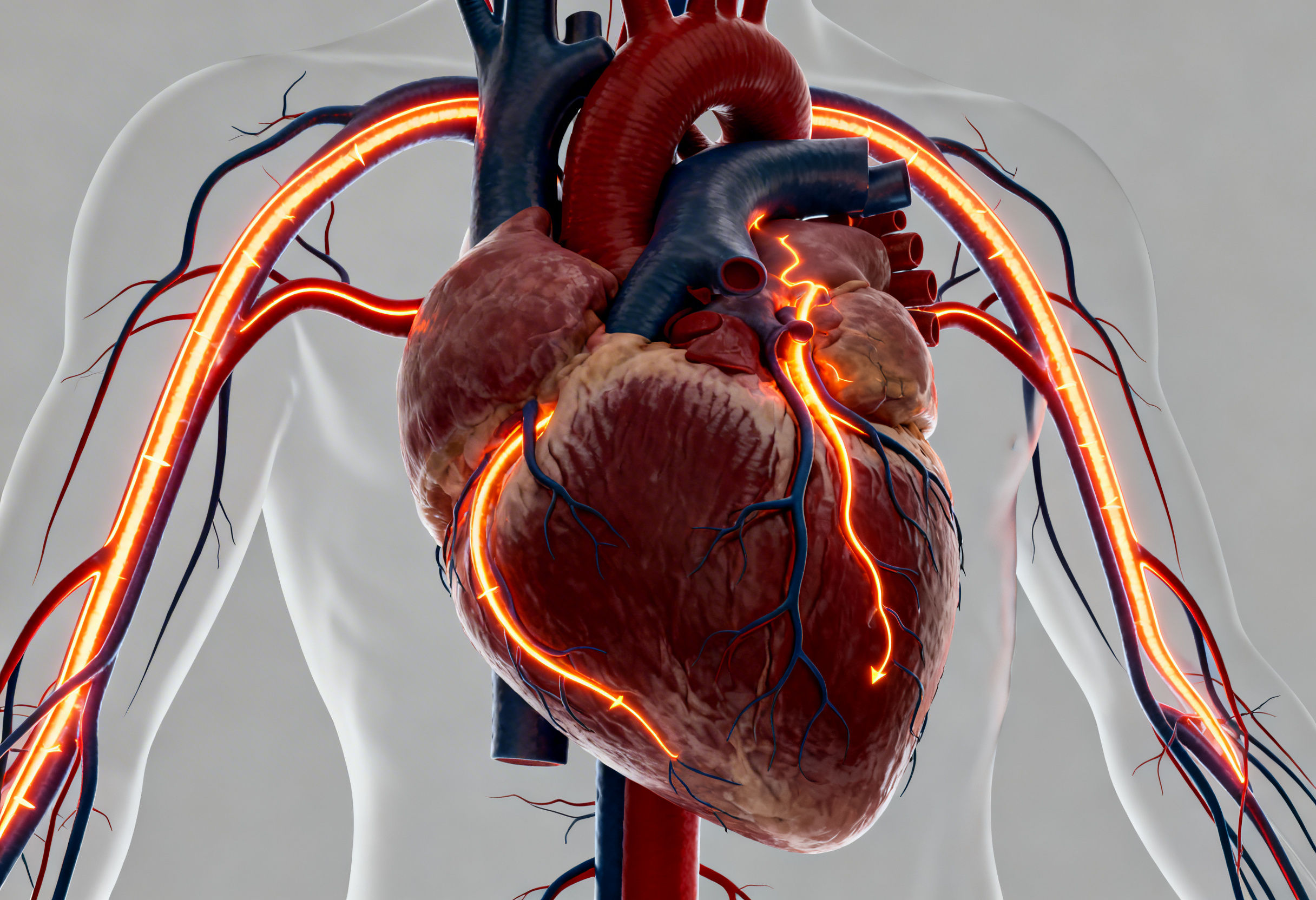
Understanding Angina: The Pathophysiology Behind Chest Pain
Angina occurs when coronary blood flow fails to meet myocardial oxygen demand. The heart extracts nearly 70 to 80 percent of oxygen from circulating blood at rest, leaving minimal reserve. Any increase in workload requires immediate vascular adaptation.
Ischemia develops due to:
- Atherosclerotic plaque formation
- Endothelial dysfunction
- Coronary microvascular impairment
- Vasospasm
During ischemia, myocardial cells shift toward anaerobic metabolism, generating lactate and stimulating nociceptive fibers, producing chest discomfort.
Types of Angina
- Stable angina – exertional and predictable
- Microvascular angina – normal large arteries but impaired small vessels
- Vasospastic angina – transient coronary spasm
- Refractory angina – persistent symptoms despite maximal therapy
ECP Therapy for angina is particularly effective in stable, microvascular, and refractory cases.
Limitations of Conventional Revascularization
Large trials such as ISCHEMIA have shown that for stable coronary artery disease, invasive procedures do not reduce mortality compared to optimal medical therapy.
Stents relieve focal obstruction but do not treat:
- Diffuse endothelial dysfunction
- Microvascular disease
- Systemic inflammation
- Plaque instability
Microvascular angina, especially common in women, often shows normal angiography results. Since there is no lesion to stent, many patients remain symptomatic without clear treatment direction.
ECP Therapy addresses these systemic vascular dysfunctions directly.
What is ECP Therapy?
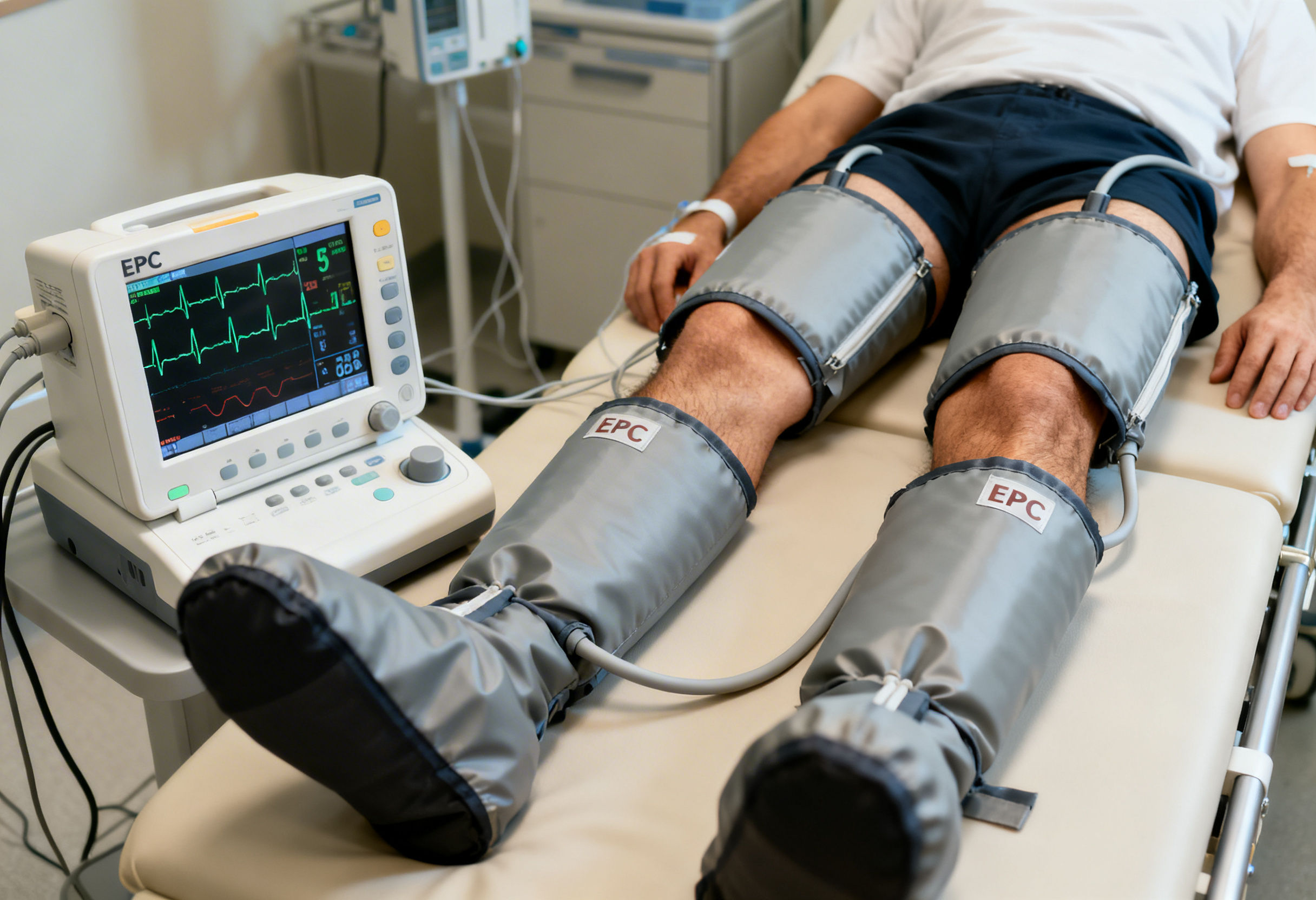
External Counterpulsation, commonly referred to as ECP or EECP, is a non-invasive cardiovascular therapy designed to enhance coronary blood flow.
It involves pneumatic cuffs wrapped around the calves, thighs, and buttocks that inflate and deflate in synchronization with the cardiac cycle.
This synchronization produces two major physiological effects:
1. Diastolic Augmentation
During diastole, the cuffs inflate sequentially from distal to proximal.
This:
- Increases aortic diastolic pressure
- Drives blood retrograde into coronary arteries
- Enhances myocardial perfusion
2. Systolic Unloading
Just before systole, cuffs deflate rapidly.
This:
- Reduces afterload
- Decreases myocardial oxygen demand
- Improves cardiac output
This dual mechanism increases oxygen supply while decreasing workload, making ECP Therapy for angina uniquely efficient.
Biological Mechanisms: Beyond Immediate Hemodynamics
The long-term benefits of ECP extend beyond session-based pressure changes.
Shear Stress and Endothelial Restoration
Increased blood flow generates shear stress on endothelial cells, stimulating:
- Nitric oxide production
• VEGF release
• Growth factor activation
• Reduction in endothelin-1
This improves vascular dilation capacity and reverses endothelial dysfunction.
Angiogenesis and Collateral Formation
Repeated treatments stimulate:
- Development of new capillary networks
• Recruitment of dormant collateral vessels
• Arteriogenesis
These newly formed channels function as natural bypasses around blocked arteries.
ECP Therapy for Microvascular Angina
Microvascular angina involves dysfunction of arterioles smaller than 500 micrometers.
Because standard angiography cannot visualize these vessels, many patients are misdiagnosed.
ECP Therapy improves perfusion across the entire vascular tree, including microvasculature. Studies show significant improvement in angina frequency and exercise tolerance in patients with INOCA.
ECP vs Angioplasty and Bypass
Feature | Angioplasty | Bypass Surgery | ECP Therapy |
Invasiveness | Moderate | High | None |
Anesthesia | Local | General | None |
Hospital Stay | 1 day | 5-7 days | Outpatient |
Mortality Risk | Low | 1-3% | None |
Recovery | Days | Weeks | Immediate |
Systemic Benefit | Limited | Limited | Yes |
ECP Therapy for angina offers symptom relief comparable to invasive procedures in stable disease without procedural risk.
Systemic Benefits of ECP Therapy
Improved Endothelial Function
Flow-mediated dilation improves after treatment, indicating systemic vascular rehabilitation.
Anti-Inflammatory Effects
ECP reduces inflammatory markers such as hs-CRP and TNF-alpha.
Autonomic Nervous System Regulation
Treatment enhances vagal tone and improves heart rate variability, shifting patients away from sympathetic dominance.
Peripheral Conditioning
Muscle oxygen extraction improves, reducing cardiac strain during exertion.

The Integrative Cardiology Model at ARKA Anugraha Hospital
ECP Therapy for angina is delivered within a broader functional medicine framework.
The Gut-Heart Axis
Elevated TMAO levels produced by certain gut bacteria promote atherosclerosis.
At ARKA, microbiome evaluation and targeted dietary strategies reduce TMAO production and systemic inflammation.
Hormonal Balance
Estrogen deficiency in women and low testosterone in men contribute to endothelial dysfunction.
Hormonal assessment ensures optimal vascular signaling.
Inflammatory Optimization
Markers such as hs-CRP, homocysteine, and oxidative stress parameters are evaluated and corrected.
This integrative approach enhances and sustains the benefits of ECP.
Who Should Consider ECP Therapy?
Ideal candidates include:
- Chronic stable angina
- Refractory angina after stents or bypass
- Microvascular angina
- Patients unsuitable for surgery
- Diabetic patients with diffuse coronary disease
Contraindications
- Severe aortic regurgitation
- Active deep vein thrombosis
- Uncontrolled arrhythmias
- Severe uncontrolled hypertension
- Pregnancy
Proper screening ensures safety.
What to Expect During Treatment
The standard course includes 35 one-hour sessions over six weeks.
Patients:
- Lie comfortably
- Experience rhythmic leg compression
- Can read or rest during therapy
- Resume normal activity immediately
Many report increased energy and reduced angina within two weeks.
Long-Term Outcomes
Clinical data shows:
- 80 to 85 percent improvement in angina class
- Sustained benefits lasting 3 to 5 years
- Reduced nitrate use
- Fewer hospital admissions
Because ECP Therapy for angina stimulates vascular remodeling, results persist beyond treatment completion.
Angina is no longer viewed solely as a mechanical obstruction problem. It is a systemic vascular dysfunction involving endothelial impairment, inflammation, and microvascular compromise.
ECP Therapy for angina offers a scientifically validated, non-surgical pathway to restore coronary perfusion, stimulate collateral circulation, and improve quality of life.
When combined with functional cardiology strategies at ARKA Anugraha Hospital, patients receive comprehensive cardiac rehabilitation that addresses both symptom and root cause.
For individuals seeking relief without surgical risk, ECP Therapy represents a powerful and evidence-based solution.
FREQUENTLY ASKED QUESTIONS
1. Is ECP Therapy safe?
Yes. It is FDA approved and non-invasive with minimal side effects.
2. How long do benefits last?
Typically 3 to 5 years depending on lifestyle factors.
3. Can I undergo ECP after bypass surgery?
Yes. It is particularly useful in post-bypass patients with recurrent symptoms.
4. Does it help microvascular angina?
Yes. It improves perfusion across small vessels.
5. Is anesthesia required?
No.
6. Can diabetics undergo ECP?
Yes, unless severe peripheral vascular disease is present.
7. Will I feel pain during therapy?
No. Pressure may feel firm but should not be painful.
8. Is ECP covered by insurance?
Coverage varies by region and policy.
9. Can it replace stents?
In stable angina, it can serve as a non-surgical alternative.
10. How soon will I feel improvement?
Many patients notice improvement within 10 to 15 sessions.
11. Does it improve heart failure?
Yes, in selected ischemic heart failure cases.
12. Are maintenance sessions needed?
Some patients benefit from periodic booster sessions.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
