ECP Therapy for Chronic Heart Failure: Can It Help Improve Your Heart Health?

- Published on: 02/March/2026
- Posted By: Arka Health

Introduction: The Silent Epidemic and the Need for Functional Restoration
Chronic Heart Failure is one of the most challenging cardiovascular disorders of modern medicine. Despite improvements in pharmacologic therapy and device-based interventions, many patients continue to experience breathlessness, fatigue, reduced exercise tolerance, and recurrent hospitalizations.
ECP therapy for chronic heart failure is increasingly being recognized as a scientifically grounded, non-invasive heart therapy that improves circulation, reduces cardiac workload, and enhances vascular health. Rather than focusing only on symptom suppression, this therapy targets perfusion deficits and endothelial dysfunction that lie at the core of heart failure pathophysiology.
At ARKA Anugraha Hospital, ECP is integrated into a broader congestive heart failure management strategy that addresses hemodynamic imbalance, mitochondrial dysfunction, and systemic inflammation.
Understanding the Pathophysiology of Chronic Heart Failure
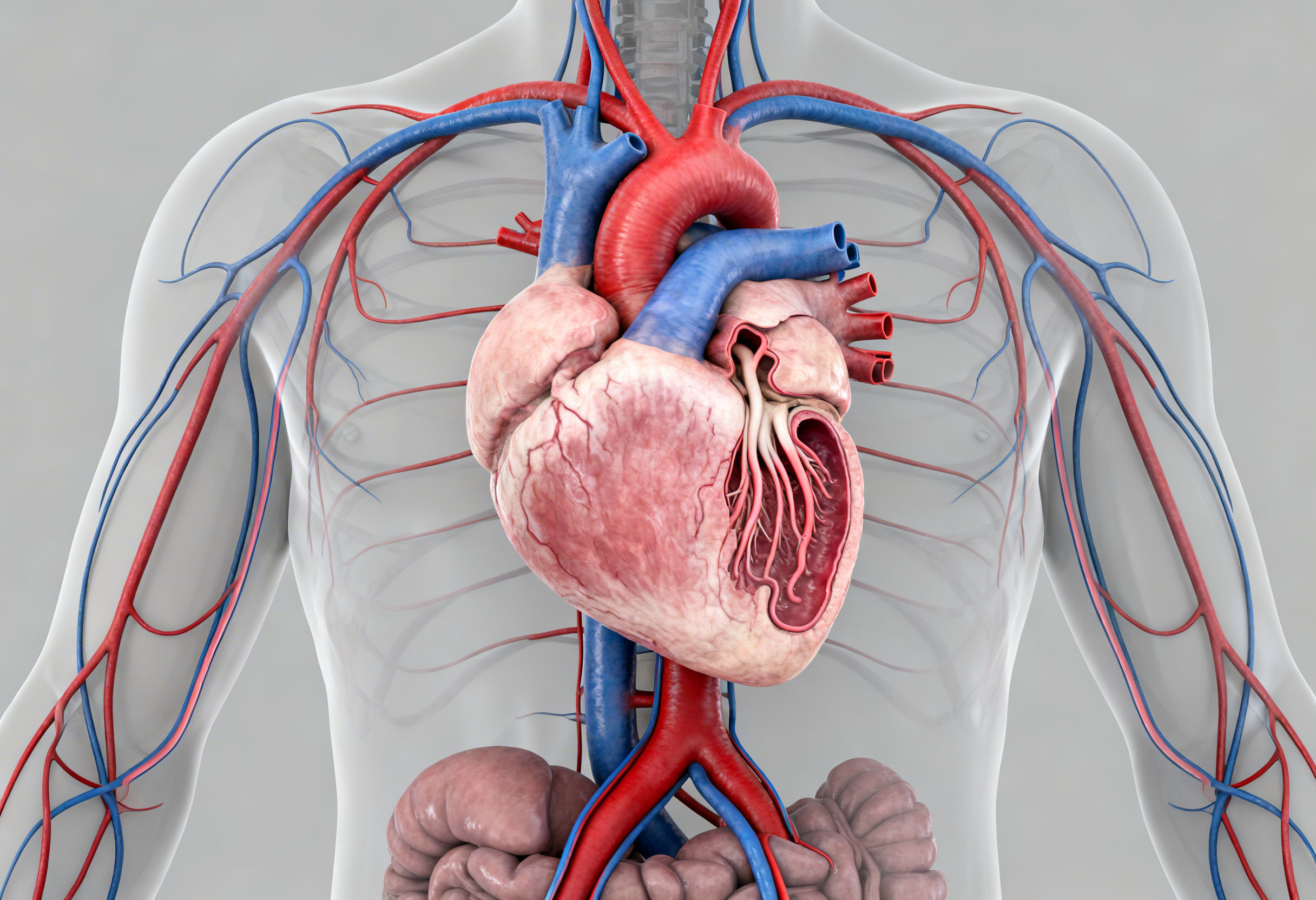
To understand how ECP therapy for chronic heart failure works, it is essential to examine the physiological derangements involved.
Forward Failure and Hypoperfusion
In Heart Failure with Reduced Ejection Fraction, systolic contractility is impaired. The left ventricle cannot eject sufficient blood, resulting in:
- Reduced systemic perfusion
- Renal hypoperfusion
- Cerebral hypoxia
- Skeletal muscle fatigue
The myocardium itself becomes energy deprived, worsening contractile dysfunction.
Backward Failure and Venous Congestion
In Heart Failure with Preserved Ejection Fraction, diastolic stiffness limits ventricular filling. Elevated left atrial pressure leads to:
- Pulmonary edema
- Orthopnea
- Peripheral edema
- Hepatic congestion
Venous congestion also affects intestinal integrity, contributing to systemic inflammation.
Neurohormonal Activation
Compensatory activation of the sympathetic nervous system and Renin Angiotensin Aldosterone System increases heart rate, vasoconstriction, and fluid retention. While initially adaptive, chronic activation promotes:
- Myocardial fibrosis
- Ventricular remodeling
- Increased afterload
- Progressive decline
Conventional medications block these pathways but do not directly improve microvascular circulation or induce vascular regeneration.
Why Standard Therapy Alone Has Limitations
Guideline directed medical therapy improves survival, but many patients remain symptomatic.
Common limitations include:
- Persistent NYHA Class II or III status
- Diuretic resistance
- Hypotension limiting dose escalation
- Ongoing endothelial dysfunction
- Poor exercise capacity
Chronic heart failure therapy must restore perfusion and reduce myocardial oxygen demand simultaneously. This is precisely where external counterpulsation heart failure treatment becomes relevant.
The Hemodynamic Science Behind ECP Therapy for Chronic Heart Failure

ECP therapy for chronic heart failure works by mechanically assisting circulation through synchronized pneumatic compression.
Diastolic Augmentation
During diastole, pneumatic cuffs inflate sequentially from calves to thighs. This produces a retrograde arterial pressure wave that:
- Increases diastolic aortic pressure
- Enhances coronary perfusion
- Improves oxygen delivery to ischemic myocardium
Since coronary blood flow predominantly occurs during diastole, this phase is critical for myocardial recovery.
Systolic Unloading
Immediately before systole, the cuffs deflate rapidly. This creates a transient reduction in peripheral vascular resistance.
The result:
- Reduced afterload
- Lower myocardial oxygen demand
- Improved stroke volume
- Increased cardiac output
This dual mechanism explains the measurable heart failure circulation improvement observed in clinical trials.
Endothelial Shear Stress and Vascular Regeneration
The long-term benefit of ECP therapy for chronic heart failure extends beyond immediate hemodynamic changes.
Nitric Oxide Enhancement
Increased pulsatile shear stress stimulates endothelial nitric oxide synthase activity. Nitric oxide:
- Promotes vasodilation
- Reduces platelet aggregation
- Improves arterial compliance
- Decreases inflammatory signaling
Improved endothelial function plays a major role in non-invasive heart therapy effectiveness.
Angiogenesis and Collateral Development
Sustained shear stress increases:
- Vascular Endothelial Growth Factor
- Basic Fibroblast Growth Factor
- Endothelial Progenitor Cell recruitment
These mechanisms stimulate angiogenesis and arteriogenesis, creating collateral vessels that function as biological bypass channels. This improves perfusion to hibernating myocardium.
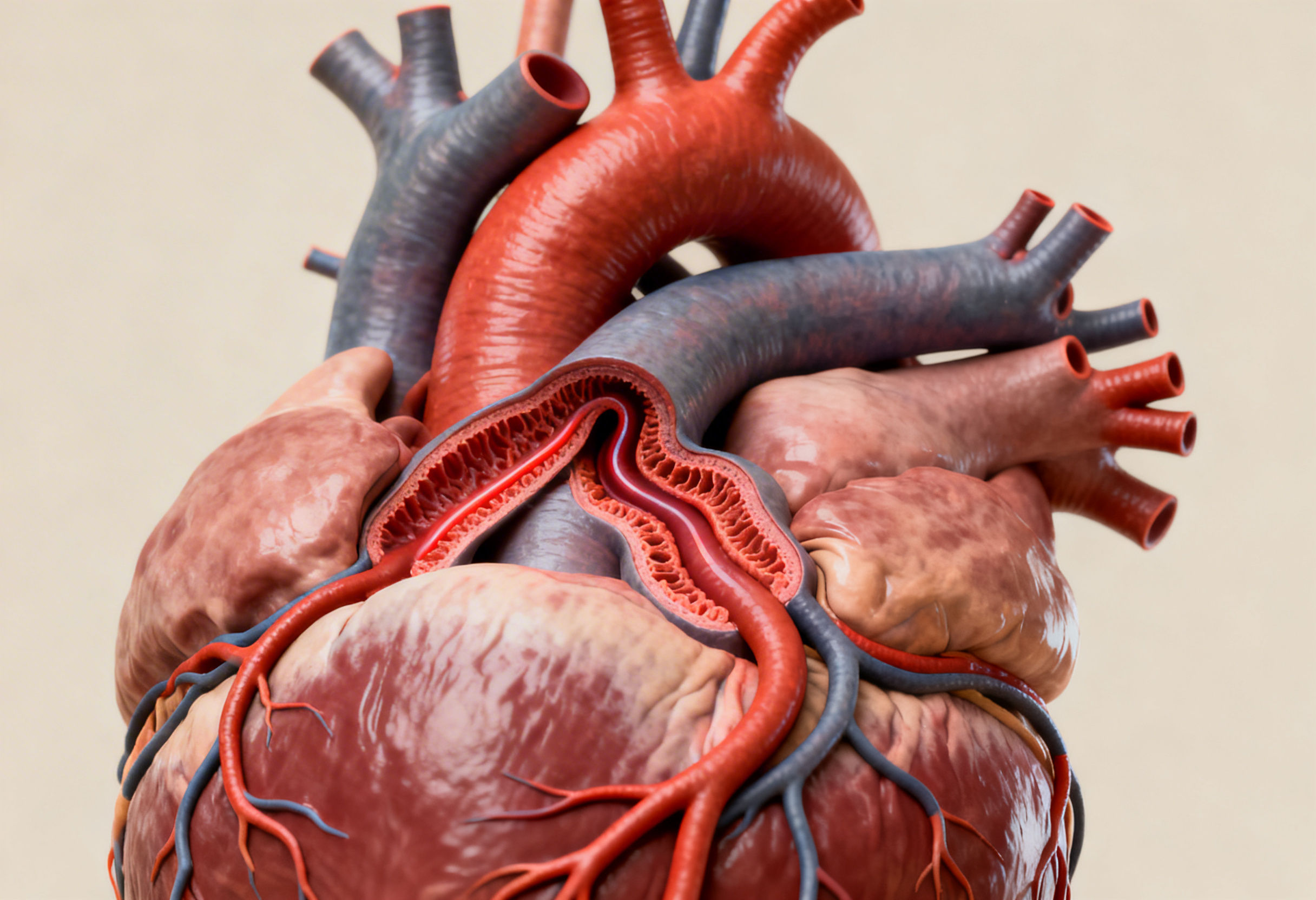
Clinical Evidence Supporting ECP Therapy
The PEECH trial evaluated ECP therapy in patients with symptomatic heart failure.
Key outcomes:
- Improved exercise duration
- Better NYHA functional classification
- Enhanced quality of life scores
- Reduced hospitalization rates
Registry data further demonstrates improved renal function and reduced emergency visits.
These findings support external counterpulsation heart failure treatment as an adjunct to standard therapy.
ECP Therapy and Cardiorenal Syndrome
Heart failure often coexists with renal dysfunction.
ECP improves renal perfusion by:
- Increasing diastolic pressure
- Enhancing renal artery blood flow
- Improving glomerular filtration rate
Studies have shown reductions in Cystatin C levels following therapy, suggesting improved kidney function. This can enhance diuretic responsiveness and reduce fluid overload.
Integrative Congestive Heart Failure Management at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, ECP therapy for chronic heart failure is combined with metabolic and functional cardiology strategies.
Mitochondrial Support
Heart failure is associated with ATP depletion. Metabolic support may include:
- Coenzyme Q10 for mitochondrial electron transport
- L Carnitine for fatty acid oxidation
- D Ribose for ATP synthesis
- Magnesium for vascular relaxation
Gut Heart Axis Support
Venous congestion can cause intestinal permeability and endotoxemia.
Dietary strategies focus on:
- Anti-inflammatory Mediterranean style nutrition
- Fiber for butyrate production
- Microbiome balance
- Reduction of pro-inflammatory metabolites
Lifestyle and Autonomic Regulation
Chronic heart failure is characterized by sympathetic dominance.
Interventions include:
- Sleep optimization
- Stress reduction techniques
- Guided breathing exercises
- Gradual supervised physical activity
This systems-based model strengthens the benefits of chronic heart failure therapy.
What to Expect During ECP Treatment
A full course consists of:
- 35 sessions
- 1 hour daily
- 5 to 6 days per week
- Approximately 6 to 7 weeks
During therapy:
- ECG synchronized cuffs inflate and deflate rhythmically
- The sensation is firm compression
- There is no anesthesia
- No recovery time is required
Many patients report improved breathing and energy levels during the treatment course.
Ideal Candidates
ECP therapy for chronic heart failure may benefit:
- NYHA Class II or III patients
- Individuals with reduced or preserved ejection fraction
- Patients not suitable for further revascularization
- Those seeking non-invasive heart therapy options
Contraindications
ECP is not suitable for:
- Severe aortic regurgitation
- Active deep vein thrombosis
- Decompensated pulmonary edema
- Severe peripheral artery disease
- Uncontrolled hypertension
Comprehensive screening ensures safety.
Long-Term Outlook

Benefits may persist for three to five years. Maintenance therapy may be considered based on clinical response.
When integrated into structured congestive heart failure management, ECP therapy for chronic heart failure offers durable improvement in functional capacity and quality of life.
FREQUENTLY ASKED QUESTIONS
- Is ECP therapy safe for elderly patients?
Yes, if properly screened and hemodynamically stable. - Can it improve ejection fraction?
Some patients show modest improvement, but functional gains are more consistent. - Does ECP replace medication?
No. It complements standard pharmacologic therapy. - How soon do improvements appear?
Many patients notice benefits within 2 to 3 weeks. - Is the treatment painful?
No, it feels like firm rhythmic compression. - Can it reduce hospital admissions?
Clinical registry data suggests reduced readmissions. - Does it help with kidney dysfunction?
Improved renal perfusion may enhance kidney function. - Can HFpEF patients benefit?
Yes, endothelial restoration can improve symptoms. - What if I miss sessions?
Consistency is important for optimal vascular remodeling. - Is anesthesia required?
No. - Can diabetics undergo ECP?
Yes, and microvascular circulation may improve. - Is it approved by cardiology guidelines?
Yes, it holds a Class IIb recommendation in specific cases. - How long do results last?
Often several years with appropriate lifestyle adherence. - Can it help exercise intolerance?
Yes, improved perfusion enhances oxygen delivery. - Is it suitable after stenting or bypass?
Yes, it can complement previous revascularization.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
