Prolotherapy for Knee Osteoarthritis: Regenerating Cartilage Without Surgery

- Published on: 23/Feb/2026
- Posted By: Arka Health
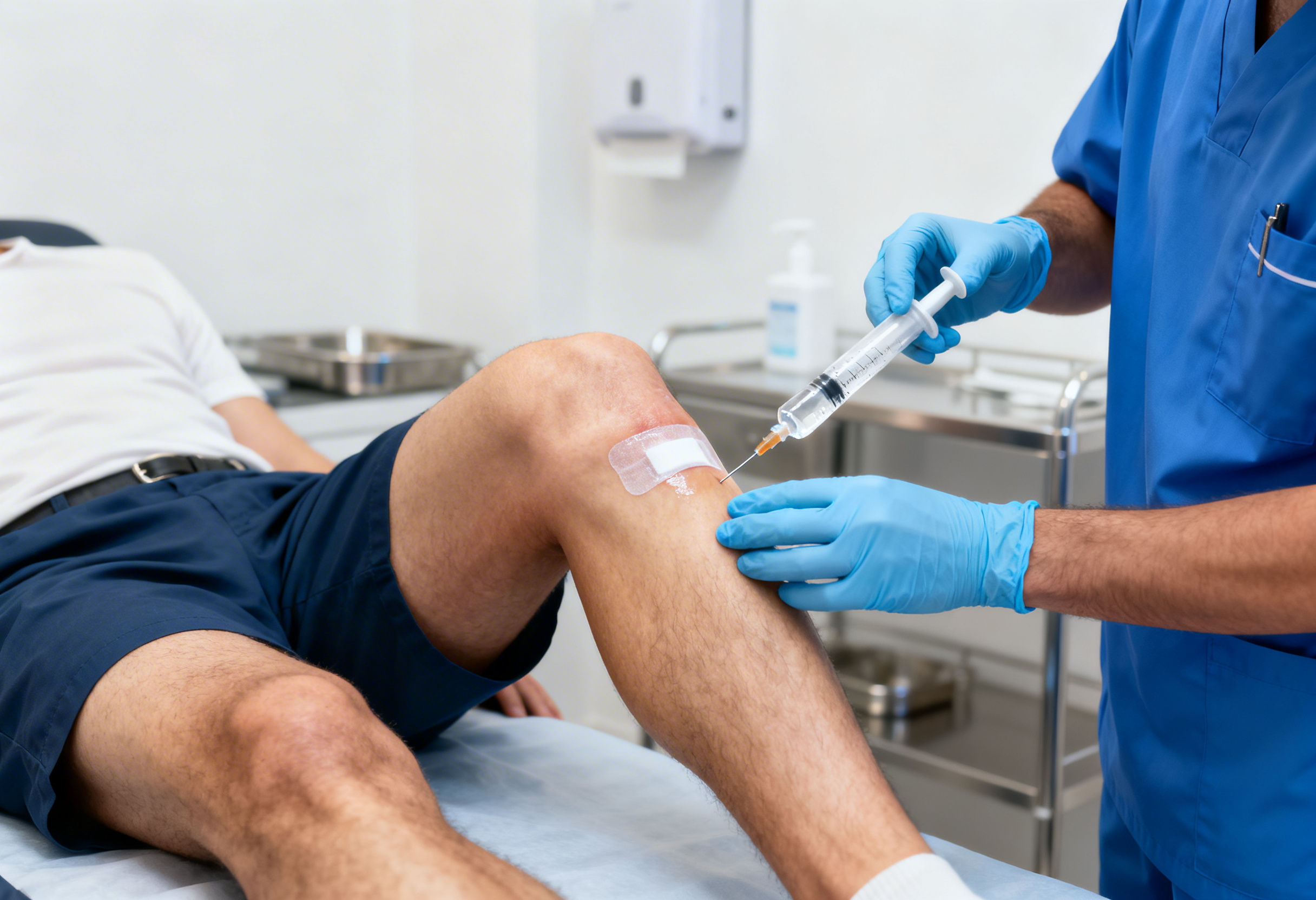
Foundational Understanding of Knee Osteoarthritis
Knee osteoarthritis is a progressive degenerative joint disorder that affects the entire joint environment rather than just the cartilage surface. It involves structural breakdown of articular cartilage, remodeling of subchondral bone, synovial inflammation, and osteophyte formation. Globally, it is one of the leading causes of disability among older adults.
Articular cartilage is a specialized avascular connective tissue composed primarily of type II collagen and proteoglycans. These components are maintained by chondrocytes, which regulate matrix turnover. In a healthy knee, cartilage distributes load evenly and allows near frictionless motion.
In osteoarthritis, the equilibrium between tissue breakdown and tissue repair shifts toward catabolism. Proteoglycan depletion reduces water retention capacity. Collagen fibers become disorganized. The cartilage softens, fissures develop, and progressive thinning follows. Over time, this may result in significant joint space narrowing and mechanical dysfunction.
However, knee osteoarthritis is not simply wear and tear. It is a biologically active disease driven by inflammatory mediators, mechanical instability, and systemic influences.
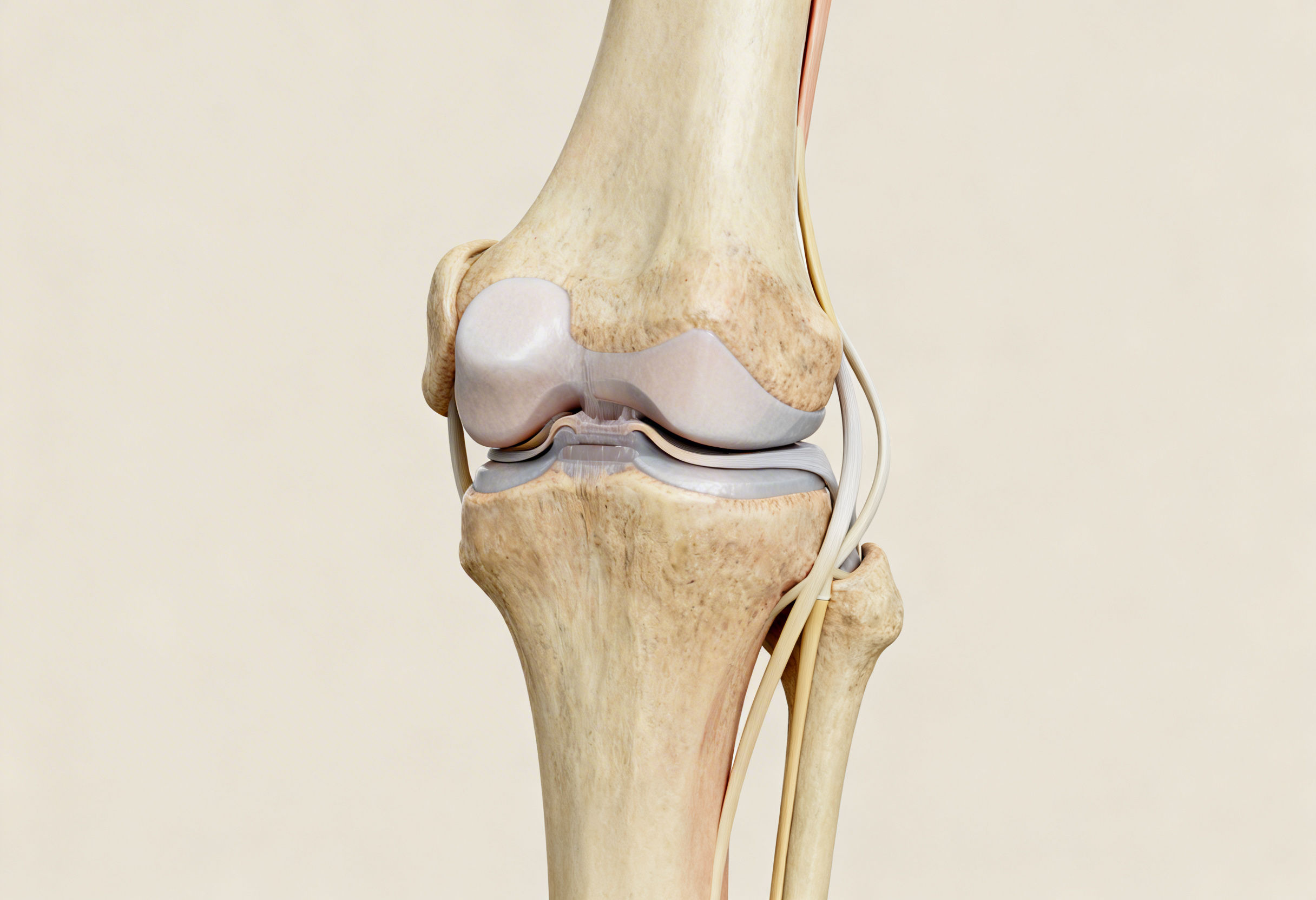
Molecular and Biomechanical Drivers of Degeneration
At the cellular level, chondrocytes undergo a phenotypic shift under chronic mechanical stress and inflammatory signaling. This leads to overexpression of matrix metalloproteinases, particularly MMP 13, and aggrecanases from the ADAMTS family. These enzymes degrade type II collagen and aggrecan, compromising cartilage resilience.
Pro inflammatory cytokines such as interleukin 1 beta and tumor necrosis factor alpha further amplify the degenerative cascade. They stimulate degradative enzyme production and induce chondrocyte apoptosis. Although transforming growth factor beta attempts repair, its effect becomes insufficient in chronic disease states.
The synovium plays a central role in symptom generation. Degraded cartilage fragments activate macrophages within synovial fluid, leading to chronic synovitis. This inflammation contributes significantly to pain perception.
Subchondral bone also remodels in response to cartilage loss. Early increased turnover may produce bone marrow lesions associated with pain. Later, sclerosis and osteophyte formation occur as compensatory stabilization mechanisms.
How Knee Osteoarthritis Progresses
Knee osteoarthritis often begins with subtle joint instability. Ligament laxity and minor untreated injuries alter load distribution. This results in focal cartilage stress and micro trauma.
Early symptoms may include intermittent discomfort, stiffness after prolonged sitting, or a sense of instability.
As degeneration progresses:
- Osteophytes develop
- Joint space narrows
- Mechanical alignment may shift
- Pain becomes more frequent
Radiographic classification such as the Kellgren Lawrence grading system tracks structural progression. However, symptom severity does not always correlate with imaging findings. Some patients with advanced radiographic changes report minimal pain, while others with mild changes experience significant functional limitation.
This discrepancy highlights the multifactorial nature of pain, including synovial inflammation, subchondral bone changes, and central sensitization.
Systemic Contributors to Knee Osteoarthritis
Modern evidence supports the view that knee osteoarthritis is influenced by systemic factors.
Metabolic Dysfunction
Adipose tissue is metabolically active. It releases adipokines such as leptin and resistin that promote cartilage degradation and inflammation. This explains why obesity increases osteoarthritis risk even in non weight bearing joints.
Hyperglycemia promotes advanced glycation end products that stiffen collagen and impair tissue elasticity.
The Gut Joint Axis
Gut dysbiosis increases intestinal permeability. Circulating endotoxins such as lipopolysaccharides activate systemic inflammatory pathways. Chronic low grade inflammation sensitizes joint tissues and worsens degeneration.
Hormonal Influence
Estrogen receptors are present in cartilage and ligament tissues. Estrogen supports collagen synthesis and has anti-inflammatory effects. Declining estrogen levels in menopause are associated with increased joint stiffness and vulnerability to degeneration.
Recognizing these systemic influences is essential when designing effective non surgical knee osteoarthritis treatment plans.
Why Conventional Treatments Often Fall Short
Traditional management strategies focus primarily on symptom suppression.
NSAIDs reduce inflammation temporarily but do not repair tissue.
Corticosteroid injections provide rapid pain relief but may inhibit chondrocyte activity and accelerate cartilage thinning when used repeatedly.
Hyaluronic acid improves lubrication but does not stimulate regeneration.
These approaches address symptoms but not structural instability or biological repair mechanisms.
This gap has led to increased interest in regenerative knee therapy approaches such as prolotherapy for knee osteoarthritis.
Prolotherapy for Knee Osteoarthritis: Biological Mechanism
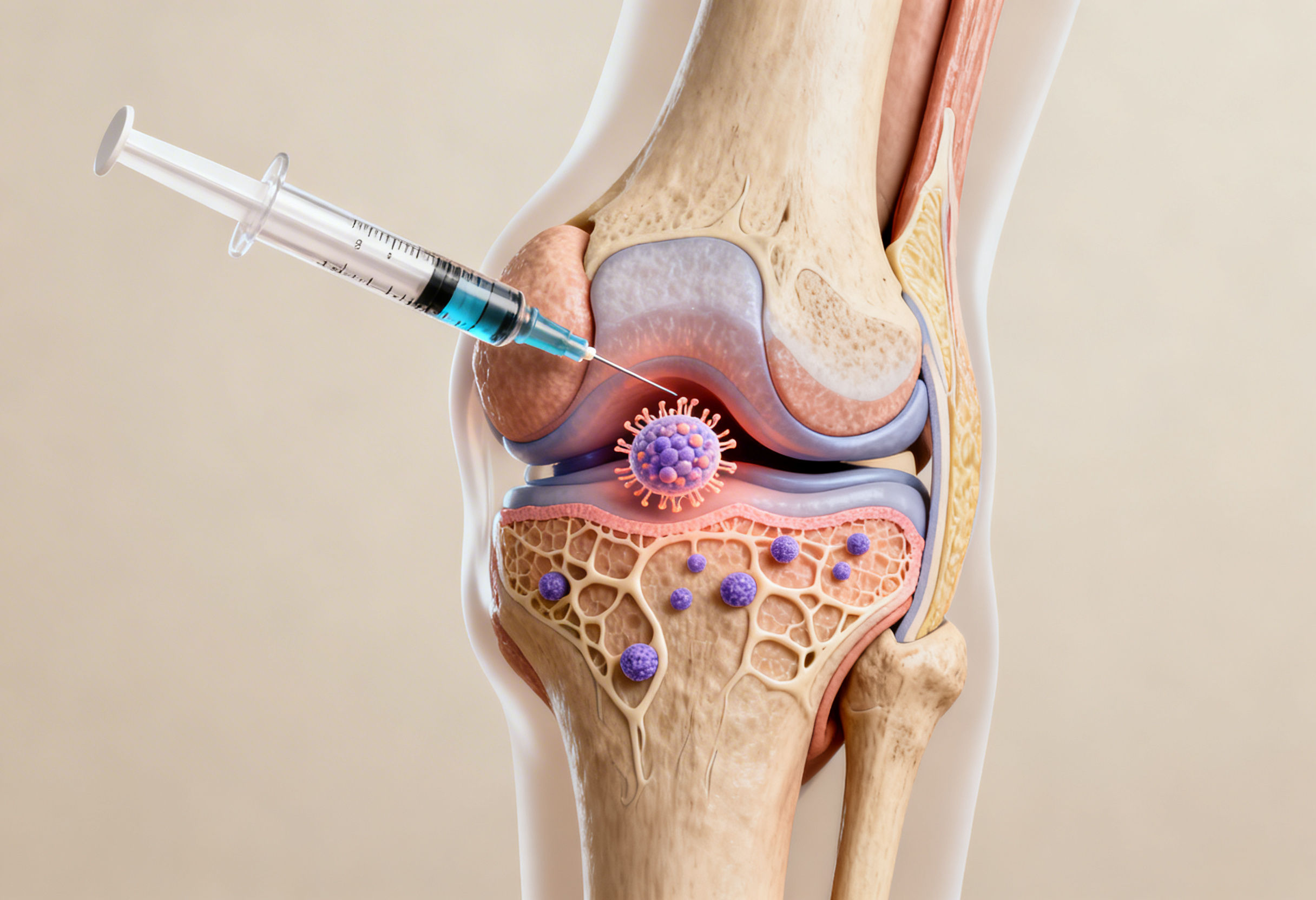
Prolotherapy is a regenerative injection therapy that uses hypertonic dextrose solution to stimulate tissue repair.
Controlled Inflammatory Activation
The injected solution creates a localized osmotic gradient, inducing mild cellular stress. This initiates an acute inflammatory response.
Macrophages are recruited and release growth factors including:
- Platelet Derived Growth Factor
• Transforming Growth Factor beta
• Insulin like Growth Factor
These growth factors stimulate fibroblast and chondrocyte activity.
Collagen and Matrix Synthesis
Fibroblasts increase collagen production at ligament and tendon insertion points. This enhances tensile strength and reduces joint laxity.
Chondrocytes increase extracellular matrix synthesis, supporting cartilage integrity.
Unlike corticosteroids, which are catabolic, prolotherapy is anabolic in nature.
Restoration of Mechanical Stability
Joint instability contributes significantly to cartilage wear. By strengthening supporting ligaments and the joint capsule, prolotherapy for knee osteoarthritis improves biomechanics and reduces abnormal shearing forces.
Improved mechanical stability reduces ongoing cartilage stress and supports long term symptom relief.
Clinical Effectiveness of Prolotherapy
Randomized clinical trials have demonstrated that prolotherapy improves:
- WOMAC pain scores
- Functional mobility
- Joint stiffness
- Patient satisfaction
While corticosteroid injections may offer superior short term relief within the first month, prolotherapy demonstrates sustained improvement at 3, 6, and 12 months.
Safety data shows minimal adverse effects, most commonly mild transient soreness.
Treatment Protocol and Recovery
A typical prolotherapy protocol involves 3 to 6 sessions spaced 4 to 6 weeks apart.
Day 1 to 3
Mild soreness or stiffness as the inflammatory phase begins.
Week 2
Proliferative phase with collagen deposition.
Week 4 to 6
Remodeling phase with increasing stability.
NSAIDs are generally avoided during early healing to preserve regenerative signaling.
Most patients resume routine activities within 24 to 48 hours.
Structural improvement becomes noticeable after the second or third session.
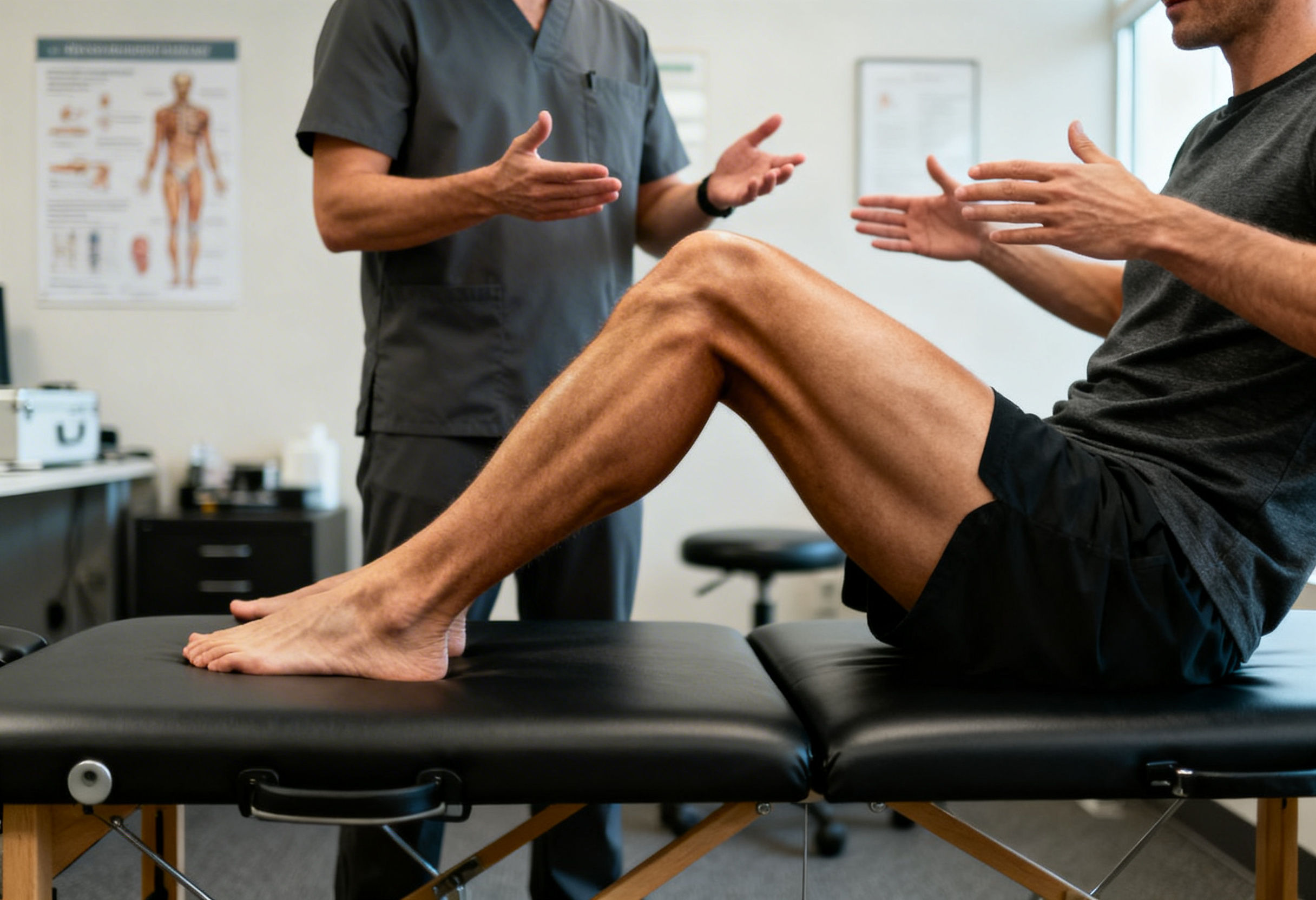
Integrative Regenerative Care at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, prolotherapy for knee osteoarthritis is delivered within an integrative systems based framework. Evaluation includes structural assessment, metabolic profiling, and inflammatory marker analysis. Dr Gaurang Ramesh and the multidisciplinary team combine regenerative injections with weight optimization, gut health correction, targeted physiotherapy, and nutritional support to enhance collagen synthesis and long term joint preservation. The objective is sustained functional recovery rather than temporary symptom control.
Long Term Clinical Relevance
Non surgical knee osteoarthritis treatment strategies that focus on regeneration can delay total knee replacement for many patients. By improving ligament stability and supporting cartilage health, prolotherapy offers a biologically grounded pathway for joint preservation.
Improved mobility contributes to better cardiovascular health, weight management, and psychological well being.
For individuals seeking cartilage regeneration injections that align with long term joint health goals, prolotherapy represents a viable regenerative knee therapy option.
FREQUENTLY ASKED QUESTIONS
- What is prolotherapy for knee osteoarthritis?
It is a regenerative injection therapy using hypertonic dextrose to stimulate collagen repair and improve joint stability. - How many sessions are required?
Most patients require 3 to 6 sessions spaced several weeks apart. - Is prolotherapy painful?
Mild temporary soreness is common but manageable. - Can prolotherapy regrow cartilage?
It stimulates matrix production and may improve cartilage integrity, though complete regrowth in advanced disease is unlikely. - Is it better than steroid injections?
Steroids suppress inflammation temporarily. Prolotherapy promotes tissue repair. - How long does improvement last?
Many patients experience sustained improvement for 12 months or longer. - Is it safe for elderly patients?
Yes, it has an excellent safety profile when administered appropriately. - Can prolotherapy delay knee replacement?
In many cases, yes, particularly in mild to moderate osteoarthritis. - Are there side effects?
Temporary stiffness and mild swelling are most common. - Can I exercise after treatment?
Light activity is encouraged. High impact exercise is gradually reintroduced. - Can prolotherapy be combined with physiotherapy?
Yes, combining regenerative injections with rehabilitation enhances outcomes. - Does weight loss improve results?
Yes, reducing joint load and systemic inflammation improves response to treatment. - Is this considered regenerative knee therapy?
Yes, because it stimulates endogenous repair mechanisms. - How soon will I notice improvement?
Some improvement may occur after the second session, with cumulative benefits over months. - Who is an ideal candidate?
Individuals with mild to moderate knee osteoarthritis seeking non surgical options.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
