ECP Therapy for Heart Attack Recovery: Accelerating Healing and Enhancing Heart Function

- Published on: 11/Feb/2026
- Posted By: Arka Health
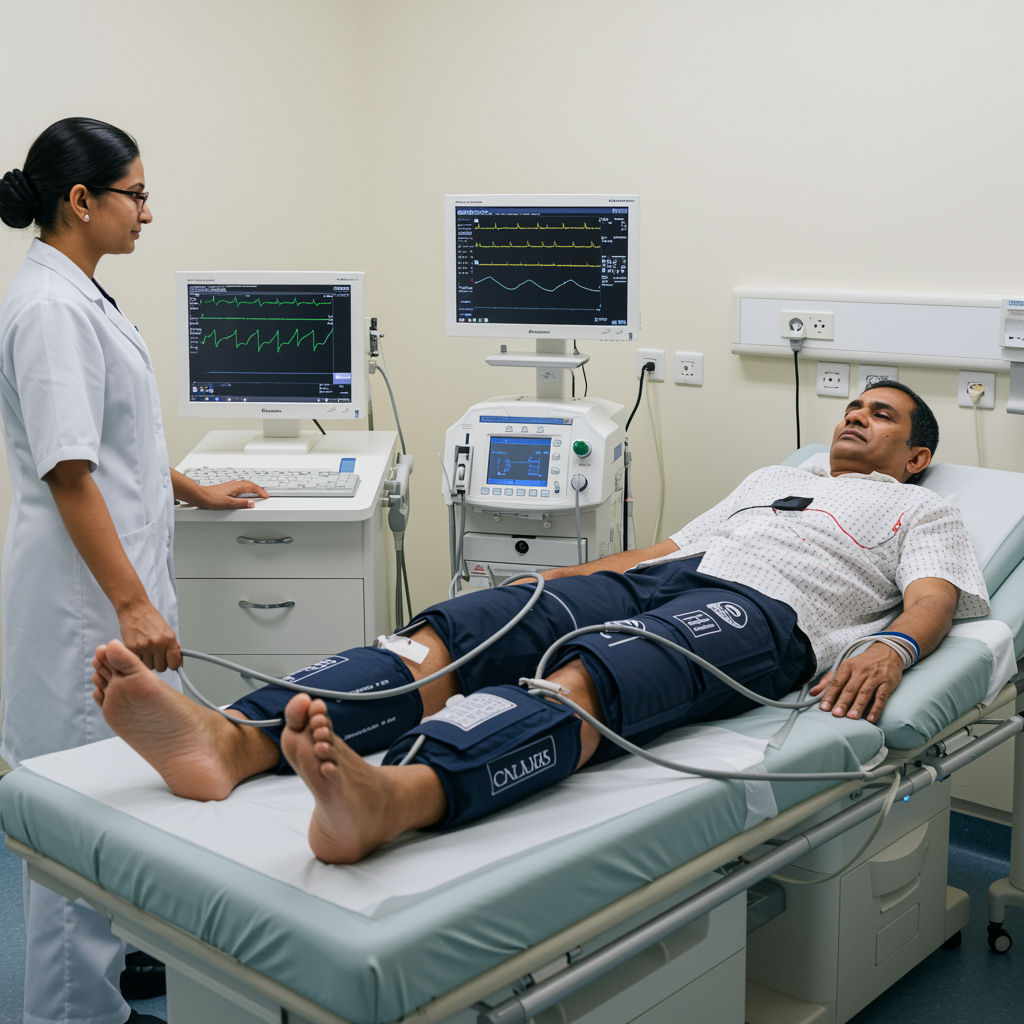
Heart attack recovery is not a single event. It is a biologically active phase in which the heart attempts to stabilize injured myocardium, restore perfusion to vulnerable regions, and prevent adverse ventricular remodeling. Even after a successful angioplasty or bypass, many patients continue to experience exertional breathlessness, fatigue, reduced exercise tolerance, and recurrent angina or angina equivalents. In a large proportion of cases, the limiting problem is not only the epicardial arteries but also persistent microvascular dysfunction, endothelial inflammation, and impaired coronary flow reserve.
Enhanced External Counterpulsation, also called ECP or EECP, is a non-invasive, outpatient therapy designed to improve coronary perfusion and reduce cardiac workload through precisely timed pneumatic compression of the lower extremities. In the context of post myocardial infarction care, ECP therapy for heart attack recovery can serve as a structured physiologic “reconditioning” program that supports myocardial oxygen delivery, improves hemodynamic efficiency, and promotes vascular repair pathways that are central to long term functional recovery.
This article explains how ECP works after a heart attack, what biological mechanisms it targets, who may benefit, and what outcomes patients can reasonably expect when it is integrated into a comprehensive rehabilitation plan.
Why Recovery After a Heart Attack Often Stalls
A myocardial infarction creates an infarct core where cardiomyocytes are lost, surrounded by a border zone of “stunned” or “hibernating” myocardium that is viable but underperfused. Early reperfusion with thrombolysis or percutaneous coronary intervention saves tissue, but it does not automatically normalize the entire coronary circulation. Many patients still have:
- Endothelial dysfunction and impaired nitric oxide signaling
- Microvascular obstruction and “no reflow” physiology in small vessels
- Diffuse atherosclerosis with multiple moderate lesions
- Residual ischemia from incomplete revascularization
- Autonomic imbalance with sympathetic predominance
- Metabolic strain from insulin resistance, diabetes, or chronic inflammation
If oxygen supply remains limited while oxygen demand remains high, the heart compensates by increasing filling pressures and neurohormonal activation. Over time, this can drive pathological remodeling, progressive decline in left ventricular function, and symptom persistence despite “successful” procedures.
ECP therapy for heart attack recovery targets this supply demand mismatch using hemodynamics first, then biology.
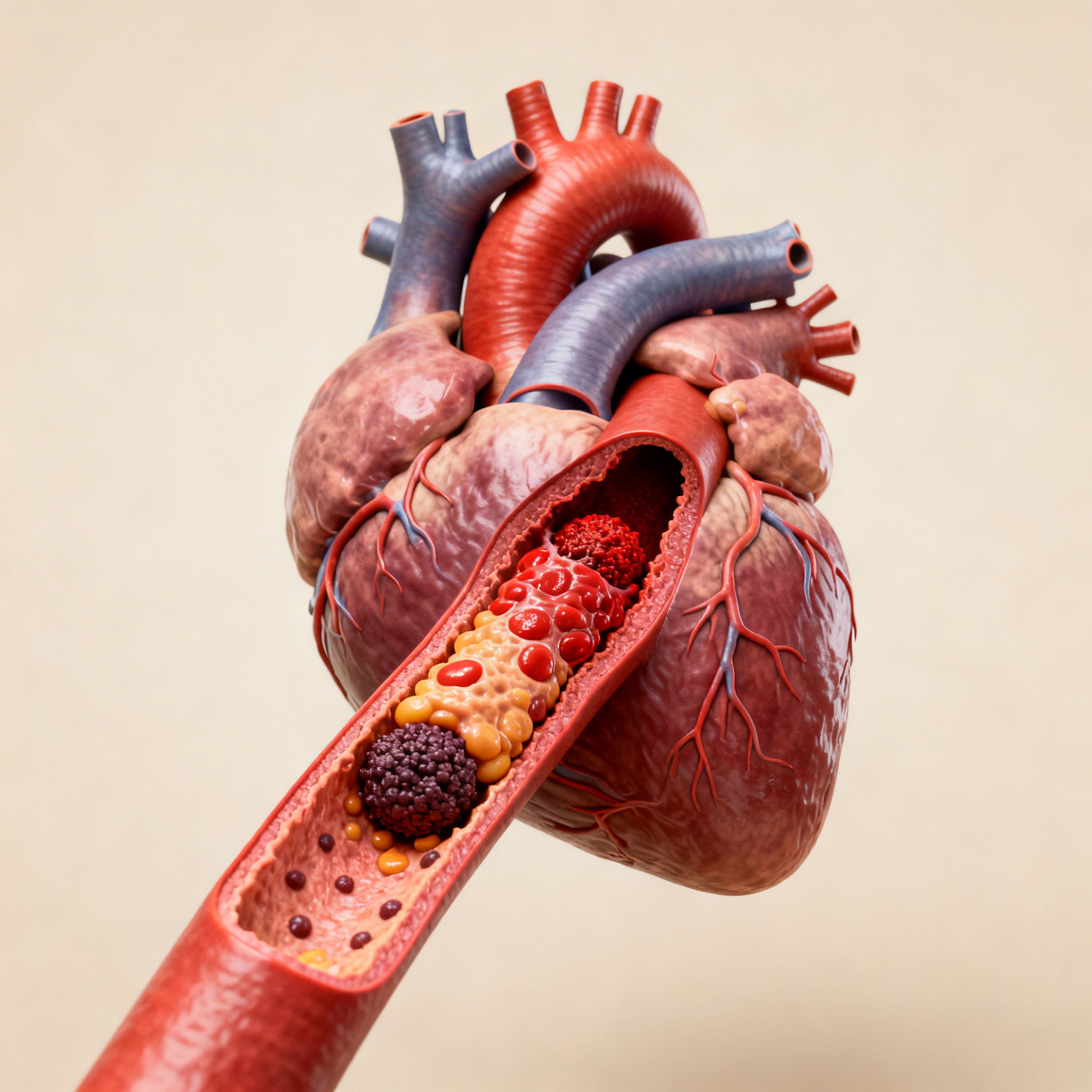
What ECP Therapy Is and How the Session Works
ECP uses three sets of pneumatic cuffs around the calves, lower thighs, and upper thighs or buttocks. The system is synchronized to the patient’s ECG so inflation and deflation occur at specific points in the cardiac cycle.
A typical session is one hour. The standard protocol commonly used in clinical practice is 35 sessions, usually five days per week for seven weeks. Patients remain awake and comfortable, with continuous monitoring of heart rhythm and hemodynamic response.
The therapy produces two core mechanical effects:
- Diastolic augmentation
- Systolic unloading
Both are directly relevant to healing after myocardial infarction.
Hemodynamic Mechanisms That Support Myocardial Healing
Diastolic augmentation: improving coronary perfusion when it matters most
Coronary blood flow predominantly occurs during diastole because systolic contraction compresses intramyocardial vessels. During ECP, cuffs inflate sequentially from distal to proximal at the onset of diastole, generating a retrograde pressure wave that increases aortic diastolic pressure. This augments coronary perfusion pressure and can increase blood flow into ischemic territories, including regions dependent on collateral supply.
For post MI patients, this matters because the border zone myocardium is often perfusion limited. Improving diastolic coronary filling supports cellular recovery, improves oxygen availability, and can reduce ischemia driven symptoms.
Systolic unloading: lowering afterload and myocardial oxygen demand
Just before systole, all cuffs deflate rapidly. This reduces peripheral vascular resistance and lowers afterload, meaning the left ventricle ejects blood against less resistance. Lower afterload decreases wall stress, reduces myocardial oxygen consumption, and improves mechanical efficiency.
This effect is particularly relevant in patients with reduced ejection fraction or those showing early remodeling patterns, where elevated wall stress perpetuates ventricular dilation.
Venous return and stroke volume support
Lower limb compression increases venous return. Through the Frank Starling mechanism, this can raise stroke volume without increasing heart rate. When balanced appropriately, it can improve cardiac output and systemic perfusion while preserving myocardial energy.
Endothelial Repair and Nitric Oxide Restoration
The endothelium is a dynamic organ that regulates vascular tone, thrombosis, and inflammation. After a heart attack, endothelial dysfunction is common due to oxidative stress, inflammation, and metabolic dysregulation.
ECP increases pulsatile shear stress, a key physiologic trigger for endothelial nitric oxide synthase activation. Improved nitric oxide availability supports:
- Vasodilation and improved flow mediated dilation
- Reduced platelet aggregation and thrombotic tendency
- Lower vascular inflammation signaling
- Improved arterial compliance
In practical terms, this can contribute to better coronary microcirculation and improved exercise tolerance, especially in patients whose angiograms do not explain their ischemic symptoms because microvascular disease is the dominant driver.
“Natural Bypass” Effects: Collateral Development and Arteriogenesis
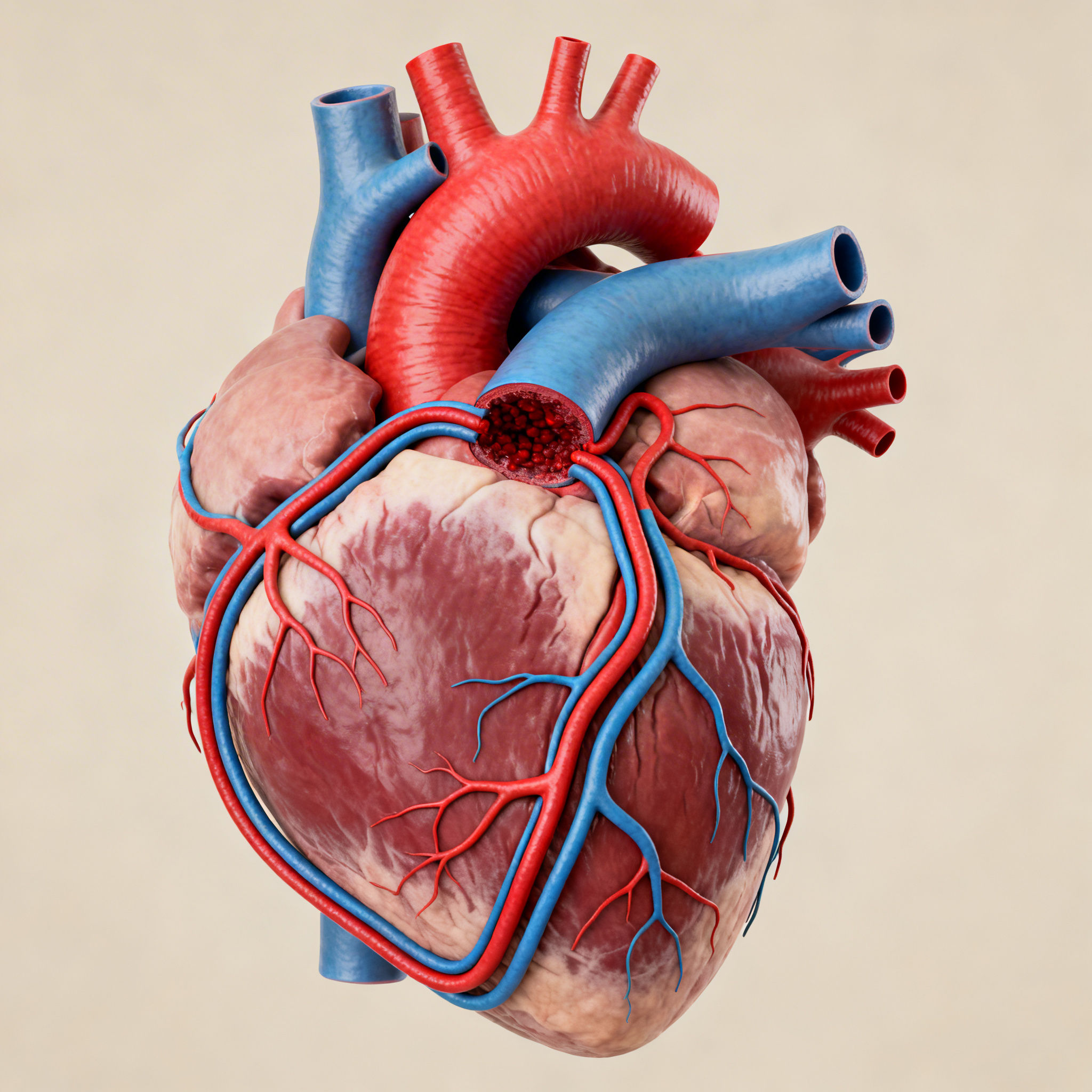
One of the most clinically meaningful long term benefits associated with ECP is promotion of collateral circulation, often described as a “natural bypass” phenomenon.
Two related processes may be supported:
Arteriogenesis:
remodeling and enlargement of pre-existing collateral arterioles into functional conductance vessels
Angiogenesis:
formation of new capillaries in response to growth factor signaling
The repeated hemodynamic stimulus over a multi week course appears to upregulate pro-angiogenic pathways, including vascular endothelial growth factor, while the mechanical pressure gradients support collateral recruitment and maturation.
This is especially valuable for patients with diffuse coronary disease, small vessel ischemia, or persistent symptoms after stent or bypass where further revascularization is limited.
Supporting Reverse Remodeling After Myocardial Infarction
Ventricular remodeling after MI includes infarct expansion, chamber dilation, and changes in myocardial geometry that increase wall stress. This progression is closely linked to long term outcomes and heart failure risk.
By reducing afterload and improving oxygen supply, ECP can act as a supportive intervention that may:
- Reduce ischemia driven neurohormonal activation
- Improve functional capacity, enabling better participation in cardiac rehabilitation
- Decrease myocardial workload during recovery windows
- Support hemodynamic conditions favorable to reverse remodeling
ECP is not a substitute for guideline directed medical therapy, but it can be an adjunct that improves the physiologic context in which medications and structured rehab work.
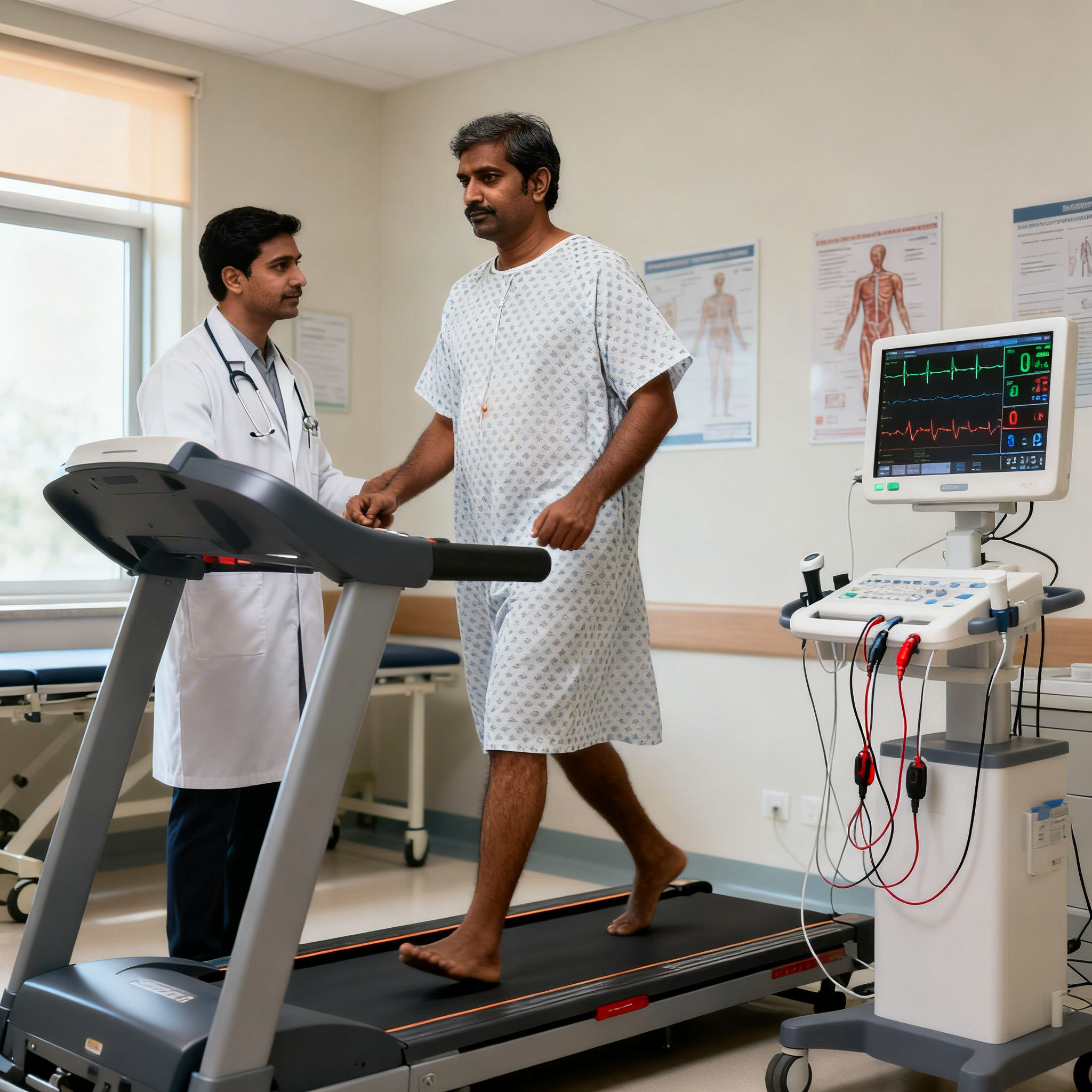
Autonomic and Inflammatory Modulation
After a heart attack, sympathetic overactivity is common and contributes to arrhythmia risk, sleep disruption, blood pressure variability, and persistent fatigue.
ECP has been associated in clinical contexts with improved autonomic balance, often discussed through improvements in heart rate variability as a marker of parasympathetic tone.
Additionally, repeated shear stress and endothelial improvements are linked with reductions in inflammatory markers such as high sensitivity C reactive protein and cytokine signaling. Lower inflammation is not only beneficial for plaque stability but also for myocardial recovery and vascular health.
Who May Benefit Most From ECP After a Heart Attack
ECP therapy for heart attack recovery is commonly considered when a patient has persistent symptoms or functional limitation despite standard care, such as:
- Ongoing angina or angina equivalents after MI
- Reduced exercise tolerance during cardiac rehabilitation
- Heart failure symptoms with ischemic substrate
- Diffuse coronary disease not suitable for further intervention
- Microvascular ischemia or INOCA patterns with objective ischemia
- High surgical risk due to age, diabetes, kidney disease, or comorbidities
- Persistent symptoms despite prior stents or bypass
ECP is typically positioned as an adjunct to medical therapy and rehabilitation, not as a replacement for emergency reperfusion strategies.
Safety, Contraindications, and Practical Considerations
ECP is generally well tolerated when patients are properly screened. Common transient issues include mild skin irritation, bruising, or fatigue early in the course, often manageable by adjusting cuff pressure and padding.
It is usually avoided in patients with:
- Active deep vein thrombosis
- Severe aortic regurgitation
- Significant uncontrolled hypertension
- Large aneurysms requiring urgent intervention
- Pregnancy
- Unstable arrhythmias that compromise synchronization
Clinical evaluation prior to initiation typically includes ECG assessment, blood pressure stability review, and vascular screening where relevant.
Integrative and Root Cause Focused Care at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, ECP therapy for heart attack recovery is best leveraged when paired with structured risk factor optimization. Heart attack recovery is strongly influenced by insulin resistance, inflammation, autonomic stress physiology, micronutrient insufficiency, sleep disruption, and medication adherence.
A systems based model integrates:
- Cardiology evaluation for ischemia burden and functional capacity
- Metabolic assessment for glucose, insulin resistance, lipids, and inflammation
- Nutrition planning focused on endothelial support and inflammation reduction
- Stress and sleep interventions to reduce sympathetic load
- Progressive rehabilitation planning so the patient can rebuild capacity safely
The goal is not only symptom reduction but improved resilience, fewer limitations in daily activity, and a more stable long term cardiovascular trajectory.
FREQUENTLY ASKED QUESTIONS
- How does ECP therapy help after a heart attack?
It increases coronary perfusion during diastole and reduces afterload during systole, improving oxygen supply while lowering cardiac workload. - Can ECP improve ejection fraction after myocardial infarction?
Some patients experience functional improvement, especially when reduced perfusion and microvascular dysfunction contribute to low performance, but results vary by infarct size and baseline LVEF. - Is ECP useful if I already had a stent or bypass?
Yes. It can help persistent symptoms by improving microcirculation and collateral flow that stents or grafts may not address. - When can ECP be started after a heart attack?
Timing depends on clinical stability and cardiology clearance. It is typically considered after the acute phase once hemodynamics are stable. - Is ECP therapy painful?
Most patients describe it as firm rhythmic compression. Discomfort is usually manageable with pressure adjustment and padding. - How many sessions are needed for ECP therapy for heart attack recovery?
A common evidence based course is 35 one hour sessions over about seven weeks. - What symptoms may improve first?
Many patients notice reduced exertional chest discomfort and better stamina around the mid course, often between sessions 15 and 25. - Does ECP reduce the risk of another heart attack?
It is not a standalone prevention strategy. Risk reduction depends on guideline directed therapy, risk factor control, and lifestyle. ECP may support vascular health as part of that plan. - Can ECP help with shortness of breath after MI?
It may help if breathlessness is related to ischemia, reduced efficiency, or heart failure physiology, especially when afterload reduction improves output. - Is ECP safe for older patients?
Often yes, and it is frequently used when surgical risk is high, provided contraindications are excluded. - Does ECP affect blood pressure?
It can influence hemodynamics during sessions. Blood pressure is monitored and hypertension should be controlled before starting. - Can diabetics benefit from ECP after a heart attack?
Yes. Endothelial improvements and microvascular support can be particularly relevant in diabetes where small vessel dysfunction is common. - Does ECP improve circulation beyond the heart?
It can improve systemic endothelial function and perfusion patterns, which is why some patients report better energy and sleep. - Can I continue normal activities after a session?
Yes. There is typically no downtime, and most patients return to routine activities immediately.
In many settings it can be repeated if symptoms recur and the patient remains an appropriate candidate after reassessment.- How does ECP therapy help after a heart attack?
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
