How ECP Therapy Improves Circulation in Patients with Peripheral Artery Disease (PAD)

- Published on: 10/Feb/2026
- Posted By: Arka Health

Peripheral artery disease is one of the most underdiagnosed vascular conditions worldwide. It affects millions of adults and significantly increases the risk of heart attack, stroke, and limb loss. Despite its prevalence, many patients ignore early warning signs such as leg heaviness or walking fatigue, assuming they are normal consequences of aging.
ECP therapy for peripheral artery disease has emerged as a non surgical approach that improves circulation by enhancing vascular function and stimulating natural collateral development. Instead of mechanically opening a single blocked artery, it rehabilitates the entire arterial network.
To understand how this works, we must first understand what peripheral artery disease does to the vascular system.
Understanding Peripheral Artery Disease
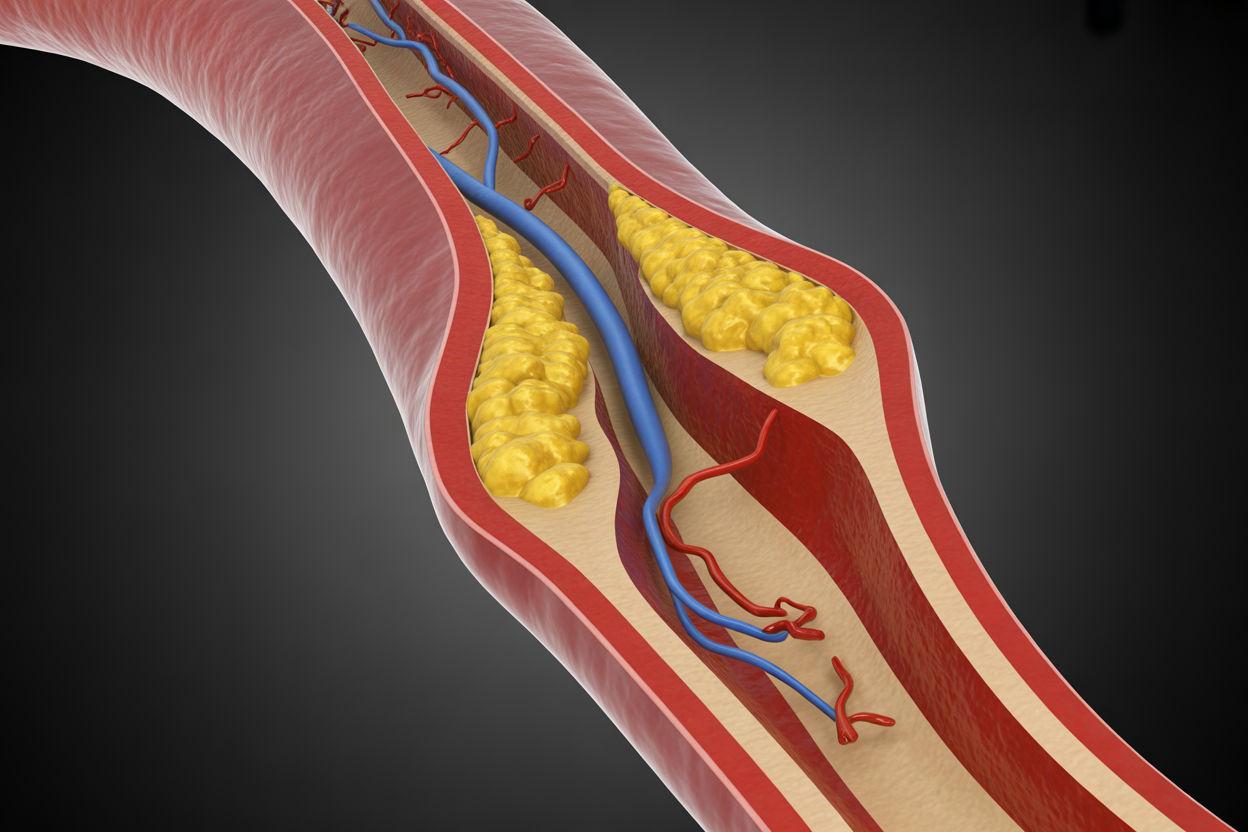
Peripheral artery disease, or PAD, is a manifestation of systemic atherosclerosis. It occurs when plaque accumulates inside the arteries that supply blood to the lower limbs.
The process begins with endothelial injury. Risk factors such as:
- Smoking
- Diabetes mellitus
- Hypertension
- Dyslipidemia
- Chronic inflammation
damage the inner lining of blood vessels. Low density lipoprotein cholesterol infiltrates the intima, becomes oxidized, and triggers an inflammatory cascade. Over time, fibroatheromatous plaques form and progressively narrow the arterial lumen.
When arterial narrowing exceeds 50 percent, blood flow becomes insufficient during exertion. The muscles of the legs require increased oxygen during walking, but stenotic arteries cannot meet demand. This leads to ischemia and the classic symptom of intermittent claudication.
Disease Progression and Collateral Failure
The body attempts compensation through collateral circulation. Small pre-existing vessels enlarge to bypass blocked arteries. At rest, these collaterals may maintain tissue viability. During exertion, however, they cannot provide adequate perfusion.
As disease progresses, patients move from:
- Exertional discomfort
- Reduced walking distance
- Rest pain at night
- Non healing ulcers
- Critical limb threatening ischemia
In advanced cases, gangrene and amputation become real risks.
ECP therapy for peripheral artery disease targets this failure of collateral compensation by stimulating vascular remodeling.
Why PAD Is Frequently Missed
Up to half of patients with PAD are asymptomatic or minimally symptomatic. Several factors contribute:
- Reduced mobility due to other illnesses
- Diabetic neuropathy masking pain
- Attribution of leg fatigue to aging
- Atypical symptom presentation in women
Because PAD is systemic atherosclerosis, ignoring leg symptoms increases the risk of cardiovascular events elsewhere in the body.
Limitations of Conventional PAD Treatments
Traditional management includes:
- Antiplatelet therapy
- Statins
- Vasodilator medications
- Supervised exercise programs
- Angioplasty or bypass surgery
While effective in selected cases, invasive interventions carry risks such as:
- Restenosis
- Surgical complications
- Wound infection
- Prolonged recovery
- Ineligibility in high risk patients
Medications may improve walking distance modestly but do not reverse endothelial dysfunction or promote robust angiogenesis.
This gap in therapy is where ECP therapy for peripheral artery disease offers a distinct advantage.
The Hemodynamic Mechanism of ECP Therapy
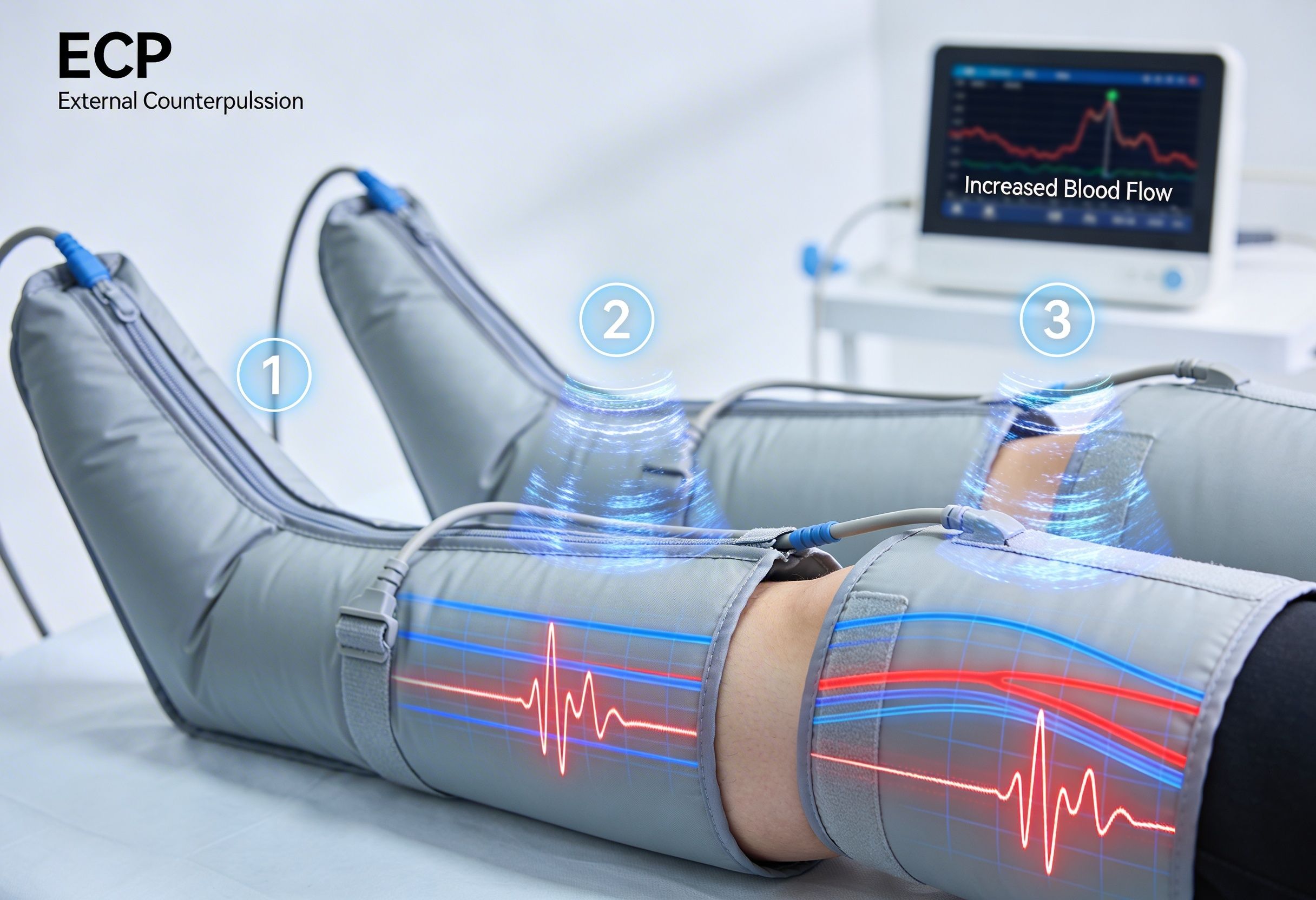
Enhanced External Counterpulsation uses pneumatic cuffs wrapped around the calves, lower thighs, and upper thighs.
The cuffs inflate and deflate in synchronization with the cardiac cycle through ECG guidance.
Diastolic Augmentation
During diastole, cuffs inflate sequentially from distal to proximal. This:
- Increases diastolic arterial pressure
- Enhances retrograde flow
- Forces blood into peripheral vascular beds
- Pushes blood into dormant collateral channels
This is critical for patients with PAD because diastolic pressure determines tissue perfusion in stenotic limbs.
Systolic Unloading
Just before systole, cuffs deflate simultaneously. This:
- Reduces systemic vascular resistance
- Decreases afterload
- Improves forward cardiac output
The combination improves net arterial flow to the lower extremities.
Endothelial Restoration
Endothelial dysfunction is central to PAD pathogenesis. Healthy endothelium produces nitric oxide, which promotes vasodilation and prevents thrombosis.
ECP therapy for peripheral artery disease increases endothelial shear stress. Shear stress stimulates endothelial nitric oxide synthase activity, leading to:
- Increased nitric oxide bioavailability
- Improved flow mediated dilation
- Reduced endothelin 1 levels
- Lower inflammatory markers
Clinical studies have demonstrated significant improvement in femoral artery endothelial function after a complete ECP course.
Angiogenesis and Arteriogenesis
One of the most powerful biological effects of ECP therapy for peripheral artery disease is stimulation of vascular growth factors.
These include:
- Vascular Endothelial Growth Factor
- Basic Fibroblast Growth Factor
- Hepatocyte Growth Factor
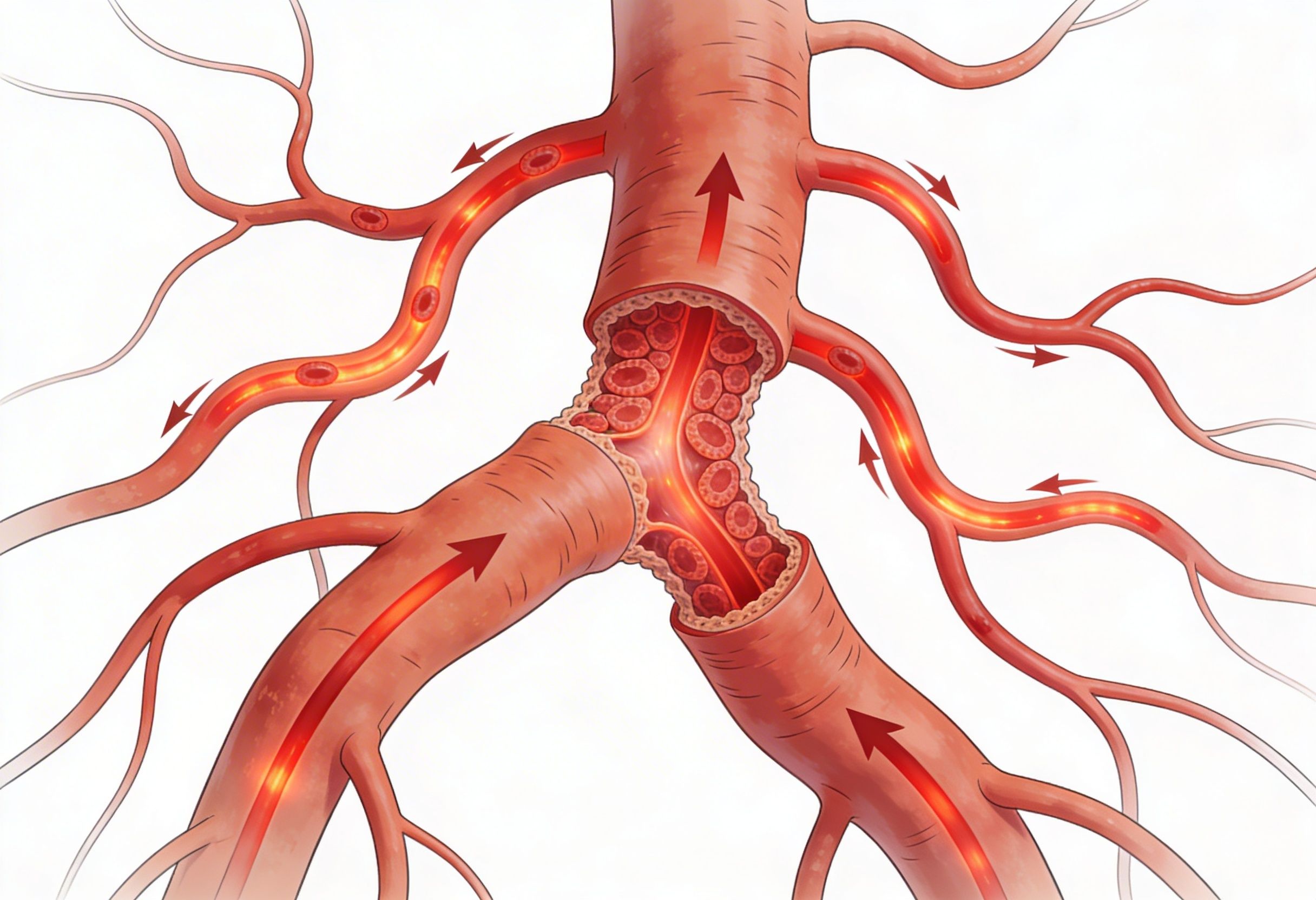
The therapy promotes:
- Angiogenesis, formation of new capillaries
- Arteriogenesis, enlargement of pre existing collateral vessels
This creates natural bypass pathways that improve sustained blood delivery to ischemic tissues.
Unlike stents, which treat a focal lesion, ECP rehabilitates the vascular network.
Reduction of Inflammation
PAD is a chronic inflammatory condition. Elevated markers such as high sensitivity C reactive protein and tumor necrosis factor alpha accelerate plaque progression.
ECP therapy has demonstrated:
- Reduction in systemic inflammatory markers
- Improved endothelial anti inflammatory signaling
- Enhanced vascular compliance
By improving the biological environment of arteries, ECP slows disease progression while enhancing circulation.
The Metabolic Component of PAD
Peripheral artery disease is rarely isolated. It is frequently associated with:
- Insulin resistance
- Type 2 diabetes
- Obesity
- Hormonal imbalance
- Gut dysbiosis
Insulin resistance damages vascular endothelium and promotes medial calcification. Gut derived metabolites such as trimethylamine N oxide accelerate atherosclerosis.
A purely mechanical approach is incomplete. Improving circulation must be combined with metabolic correction.
Treatment Protocol and Patient Experience
A standard ECP therapy course consists of:
- 35 sessions
- One hour per session
- Five days per week
- Approximately seven weeks
Patients lie comfortably while rhythmic compression occurs. The sensation resembles firm massage. There is no anesthesia and no recovery time.
Many patients begin noticing improved walking distance around sessions 15 to 20.
Clinical Benefits Observed
Patients undergoing ECP therapy for peripheral artery disease commonly report:
- Increased claudication distance
- Reduced rest pain
- Improved wound healing
- Better lower limb warmth
- Increased overall energy
Durability of results may extend three to five years, particularly when lifestyle modification accompanies therapy.

Integrative Vascular Care at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, ECP therapy for peripheral artery disease is delivered within a comprehensive vascular care framework.
The approach includes:
- Detailed vascular assessment
- Metabolic risk profiling
- Inflammation evaluation
- Personalized ECP protocols
- Nutritional and lifestyle intervention
The objective is not only PAD pain relief but systemic cardiovascular risk reduction. By combining hemodynamic therapy with metabolic stabilization, long term outcomes improve significantly.
Safety and Eligibility
ECP therapy is safe for most patients when properly screened.
Contraindications include:
- Active deep vein thrombosis
- Severe aortic regurgitation
- Large unstable aneurysm
- Pregnancy
- Uncontrolled hypertension
Proper cardiovascular evaluation ensures safe initiation.
FREQUENTLY ASKED QUESTIONS
- How does ECP therapy for peripheral artery disease improve circulation?
It increases diastolic pressure and stimulates collateral vessel development, enhancing blood delivery to ischemic limbs. - Is ECP therapy painful?
No. Most patients describe rhythmic compression similar to a deep tissue massage. - Can it replace bypass surgery?
In selected patients, yes. It is especially useful in those not suitable for invasive procedures. - How long do benefits last?
Often three to five years when combined with lifestyle management. - Can it help diabetic patients with PAD?
Yes. It improves endothelial function and may enhance microvascular perfusion. - Does it reduce amputation risk?
Improved perfusion may reduce progression to critical limb threatening ischemia. - Is it safe for elderly patients?
Yes, after proper screening. - Can I undergo ECP after a stent?
Yes. It may improve surrounding vascular health. - How many sessions are needed?
Typically 35, though complex cases may require more. - Is there downtime after treatment?
No. Patients resume daily activities immediately. - Does ECP lower inflammation?
Yes. It reduces inflammatory markers and improves endothelial function. - Can it improve walking distance?
Yes. Many patients report significant improvement in claudication threshold. - Is insurance coverage available?
Coverage depends on indication and policy terms. - Does it help heart health as well?
Yes. It reduces cardiac workload and supports systemic vascular function.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
