ECP Therapy for Stroke Recovery: Can It Aid in Rehabilitation?

- Published on: 09/Feb/2026
- Posted By: Arka Health
Stroke is a leading cause of long-term neurological disability worldwide. While advances in thrombolysis and mechanical thrombectomy have improved acute survival, many survivors are left with persistent deficits affecting mobility, speech, cognition, and independence. Traditional rehabilitation focuses on physiotherapy, occupational therapy, and speech retraining to harness neuroplasticity. However, these efforts often reach a functional plateau when cerebral perfusion remains suboptimal.
ECP therapy for stroke recovery is increasingly being explored as a hemodynamic adjunct to rehabilitation. By enhancing cerebral blood flow and improving vascular function without invasive procedures, Enhanced External Counterpulsation offers a circulatory foundation that may amplify neurological recovery.
What Is Enhanced External Counterpulsation?
Enhanced External Counterpulsation, commonly abbreviated as ECP or EECP, is a non-surgical therapy originally developed for refractory angina and ischemic heart disease.
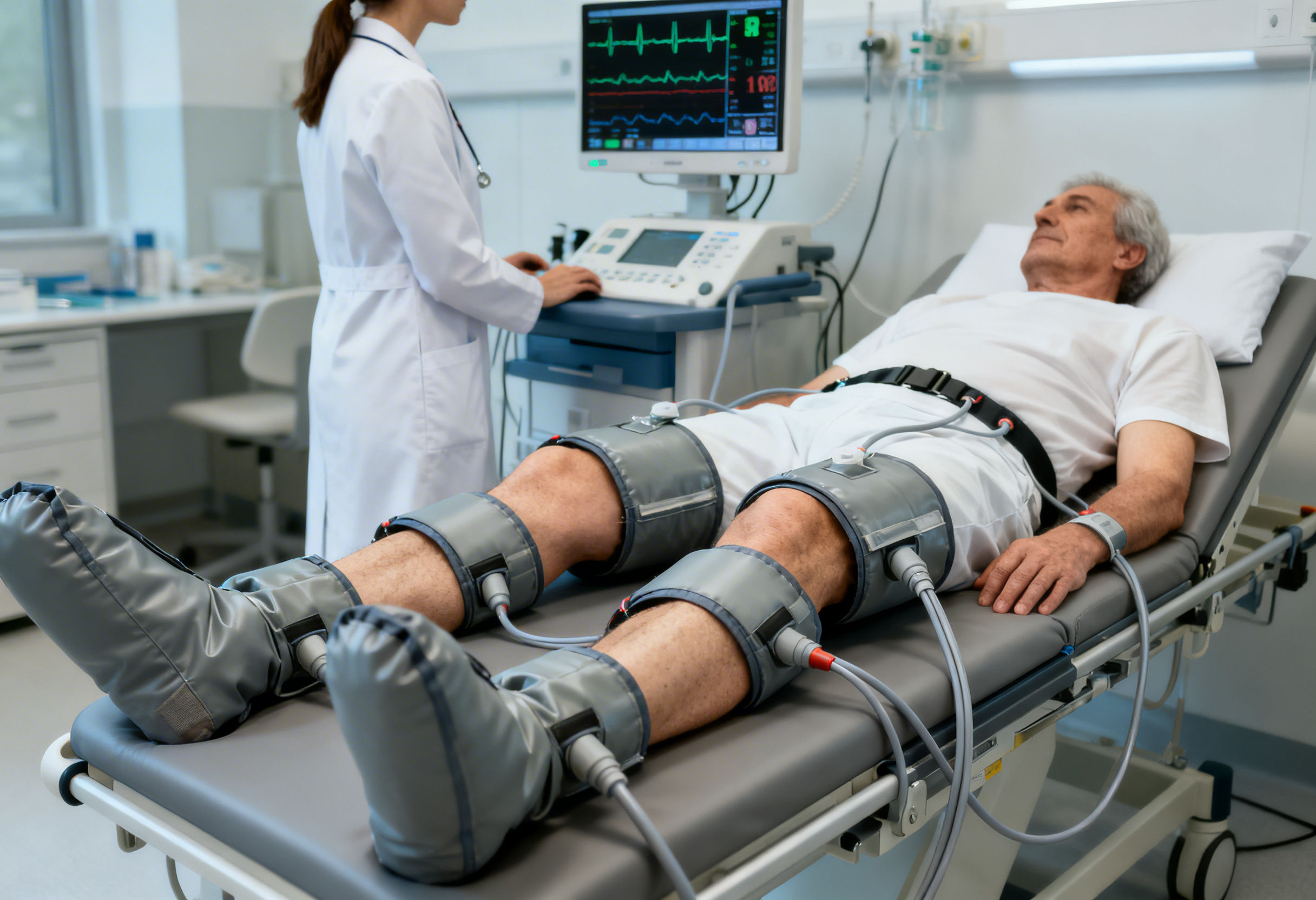
The treatment involves:
- Three sets of pneumatic cuffs wrapped around the calves, lower thighs, and upper thighs
- Continuous ECG synchronization
- Sequential inflation and rapid deflation aligned with the cardiac cycle
The therapy acts as a mechanical circulatory assist device, augmenting blood flow during diastole and reducing cardiac workload during systole.
The Hemodynamic Principle Behind ECP
ECP therapy for stroke recovery works through two primary mechanisms.
1. Diastolic Augmentation
During diastole, when the heart relaxes, the cuffs inflate sequentially from distal to proximal. This creates:
- Retrograde arterial pressure waves
- Increased diastolic pressure
- Enhanced perfusion of the coronary and cerebral arteries
Since cerebral circulation is partially dependent on diastolic pressure, this augmentation increases blood delivery to hypoperfused brain regions.
2. Systolic Unloading
Just before systole, all cuffs deflate simultaneously. This results in:
- Reduced systemic vascular resistance
- Decreased afterload
- Lower myocardial oxygen demand
The net effect is improved cardiac efficiency and increased forward flow to the brain.
Stroke Pathophysiology and the Role of Perfusion
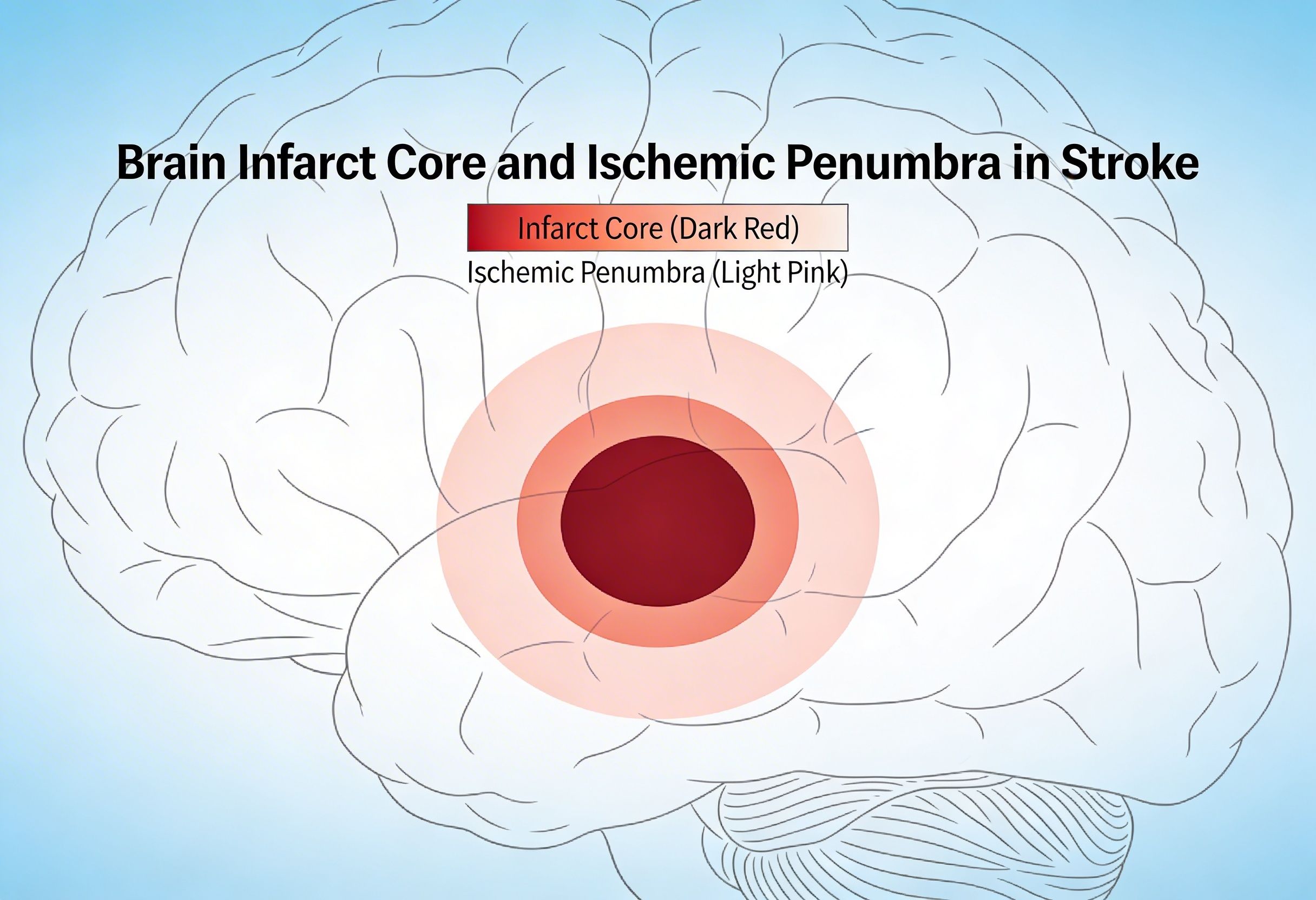
Ischemic stroke occurs when cerebral blood flow falls below the threshold required for neuronal survival. The affected region consists of:
- The infarct core, where irreversible cell death occurs
- The ischemic penumbra, a zone of metabolically stressed but salvageable tissue
Rehabilitation depends on preserving and reactivating the penumbra. However, post-stroke microvascular dysfunction often limits perfusion even after primary vessel recanalization.
The No-Reflow Phenomenon
Even after clot removal, capillary beds may remain constricted due to:
- Endothelial swelling
- Microthrombi
- Inflammatory cell infiltration
This persistent hypoperfusion restricts oxygen delivery and impairs neuroplasticity.
ECP therapy for stroke recovery attempts to overcome this microvascular resistance by increasing diastolic pressure and improving collateral circulation.
Effects on Cerebral Blood Flow
Studies using transcranial Doppler and imaging modalities have shown that counterpulsation therapy can increase mean blood flow velocity in:
- The middle cerebral artery
- The internal carotid artery
Reported improvements range from 20 percent to 40 percent during active sessions. This transient increase in perfusion may provide critical metabolic support to vulnerable neural tissue.
Endothelial Shear Stress and Vascular Repair
One of the most important biological effects of ECP is increased endothelial shear stress.
As blood flow surges during diastole, shear forces stimulate endothelial cells to produce:
- Nitric oxide
- Vascular Endothelial Growth Factor
- Anti-inflammatory mediators
Nitric Oxide
Nitric oxide promotes:
- Vasodilation
- Inhibition of platelet aggregation
- Improved microvascular flexibility
Stroke patients frequently exhibit endothelial dysfunction. Enhancing nitric oxide bioavailability may restore vascular responsiveness.
Angiogenesis
Shear stress also induces angiogenesis. The development of new capillaries may improve perfusion to chronically hypoxic brain regions, supporting long-term recovery.
Neuroplasticity and Brain-Derived Neurotrophic Factor
Recovery after stroke depends on neuroplasticity, the brain’s ability to reorganize neural networks.
Neuroplastic processes require:
- Adequate oxygen
- Glucose supply
- Neurotrophic signaling
ECP therapy for stroke recovery has been associated with increased levels of Brain-Derived Neurotrophic Factor. BDNF supports synaptic remodeling and neuron survival.
Improved perfusion combined with neurotrophic stimulation may create a favorable biological environment for functional rehabilitation.
Clinical Manifestations That May Benefit
Stroke survivors commonly experience:
Motor Deficits
- Hemiparesis
- Impaired coordination
- Spasticity
Improved perfusion may enhance motor cortex activation and responsiveness to physiotherapy.
Cognitive Impairment
- Reduced executive function
- Memory deficits
- Attention disturbances
By improving cerebral circulation, ECP may reduce cognitive fatigue and support cortical recovery.
Chronic Fatigue
Post-stroke fatigue is often linked to persistent hypoperfusion. Augmenting circulation may improve systemic and cerebral energy availability.
Why Recovery Plateaus Occur
Many patients are told that recovery stabilizes after six months. While early recovery is rapid, the brain retains plastic potential for years.
Plateaus often result from:
- Inadequate cerebral perfusion
- Chronic inflammation
- Reduced cardiac output
- Metabolic dysfunction
ECP therapy for stroke recovery addresses the hemodynamic component that is frequently overlooked.
The Brain-Heart Axis
Stroke and heart disease are closely interconnected.
- Atrial fibrillation increases embolic stroke risk
- Left ventricular dysfunction reduces cerebral perfusion
- Autonomic imbalance affects vascular tone
Improving cardiac output and vascular compliance through counterpulsation enhances the overall circulatory support available to the brain.
Comparison with Traditional Rehabilitation
Approach | Primary Mechanism | Effect on Perfusion |
Physiotherapy | Motor relearning | Indirect |
Medication | Antithrombotic prevention | Minimal |
ECP Therapy | Hemodynamic augmentation | Direct increase |
ECP does not replace physiotherapy. Instead, it provides a circulatory platform that may improve responsiveness to conventional therapy.

Treatment Protocol
A standard ECP therapy course consists of:
- 35 one-hour sessions
- Five days per week
- Approximately seven weeks total
What Patients Experience
- Rhythmic compression sensation in the legs
- Continuous ECG monitoring
- No anesthesia
- No recovery downtime
Most patients resume daily activities immediately after sessions.
Safety and Eligibility
ECP therapy for stroke recovery is generally safe when properly screened.
Contraindications include:
- Active deep vein thrombosis
- Severe aortic regurgitation
- Large unstable aneurysm
- Uncontrolled hypertension
- Pregnancy
Careful cardiovascular evaluation is essential before initiation.
Integrative Stroke Rehabilitation at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, ECP therapy for stroke recovery is integrated within a systems-based rehabilitation model.
The approach includes:
- Cardiovascular assessment
- Metabolic optimization
- Nutritional support
- Inflammation control
- Coordinated physiotherapy
By combining hemodynamic support with metabolic stabilization, the aim is to optimize the internal environment for neural recovery.
Expected Timeline of Improvement
While individual responses vary, patients often report:
Weeks 1 to 2
Improved sleep and energy levels.
Weeks 3 to 5
Better mental clarity and endurance.
Weeks 6 to 7
Enhanced mobility, coordination, and functional independence.
Benefits may persist for several years, especially when combined with lifestyle and risk factor modification.
FREQUENTLY ASKED QUESTIONS
- Can ECP therapy help years after a stroke?
Yes. Chronic hypoperfusion may persist long after the acute event. Improving circulation can support delayed neuroplasticity. - Is ECP therapy painful?
No. Most patients describe it as rhythmic pressure similar to a firm massage. - Does it replace physiotherapy?
No. It enhances the physiological environment to improve rehabilitation outcomes. - How does ECP improve cerebral circulation?
It increases diastolic pressure, pushing blood into cerebral arteries and collateral vessels. - Is there downtime after sessions?
No. Patients resume normal activities immediately. - Can it reduce stroke recurrence?
By improving vascular function and endothelial health, it may reduce long-term risk when combined with standard preventive care. - Does ECP dislodge plaques?
No evidence suggests increased plaque rupture risk. - Who benefits most?
Patients with ischemic stroke, persistent fatigue, cognitive impairment, or rehabilitation plateau. - Is it suitable for elderly patients?
Yes, after appropriate cardiovascular screening. - Can it help speech recovery?
Improved perfusion may support cortical regions involved in language. - What is the duration of benefit?
Often three to five years, depending on risk factor management. - Does insurance cover ECP?
Coverage depends on diagnosis and provider policies. - Can it be repeated?
Yes, booster sessions may be considered if symptoms recur.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
