ECP Therapy for Diabetic Heart Disease: How It Helps Improve Circulation and Blood Flow

- Published on: 04/Feb/2026
- Posted By: Arka Health
The coexistence of Type 2 diabetes and cardiovascular disease represents one of the most serious global health challenges today. Diabetic heart disease is not simply heart disease occurring in a patient with high blood sugar. It is a complex vascular and myocardial disorder driven by chronic hyperglycemia, insulin resistance, endothelial dysfunction, and diffuse microvascular injury.
ECP therapy for diabetic heart disease has emerged as a non-invasive strategy that improves circulation, enhances myocardial perfusion, and supports metabolic stability without surgical trauma. For patients who are high risk surgical candidates or who have persistent symptoms despite stents or bypass, ECP provides a physiologically sound alternative.
The Pathophysiology of Diabetic Heart Disease
Diabetic heart disease develops through intertwined metabolic and vascular pathways.
1. Chronic Hyperglycemia and Advanced Glycation
Persistently elevated glucose levels lead to the formation of advanced glycation end products. These molecules accumulate in the vascular wall and myocardium, causing:
- Increased arterial stiffness
• Oxidative stress
• Activation of inflammatory cytokines
• Reduced nitric oxide bioavailability
Nitric oxide is essential for vasodilation and endothelial protection. Its depletion results in impaired coronary perfusion and a pro thrombotic environment.
2. Diffuse Microvascular Dysfunction
Unlike focal coronary artery disease, diabetes causes diffuse injury affecting:
- Large epicardial arteries
• Small resistance vessels
• Capillary networks
Capillary rarefaction reduces oxygen delivery to myocardial tissue, even when angiography shows no critical blockage. This explains why many diabetic patients develop ischemic symptoms without significant single vessel obstruction.
3. Diabetic Cardiomyopathy
Diabetic cardiomyopathy is characterized by:
- Early diastolic dysfunction
• Myocardial fibrosis
• Left ventricular hypertrophy
• Reduced compliance
The heart becomes stiff and inefficient. Because autonomic neuropathy blunts pain perception, many patients experience silent ischemia.
Symptoms may present as:
- Shortness of breath
• Fatigue
• Reduced exercise tolerance
• Leg swelling
By the time symptoms become obvious, structural remodeling may already be advanced.
How ECP Therapy for Diabetic Heart Disease Works
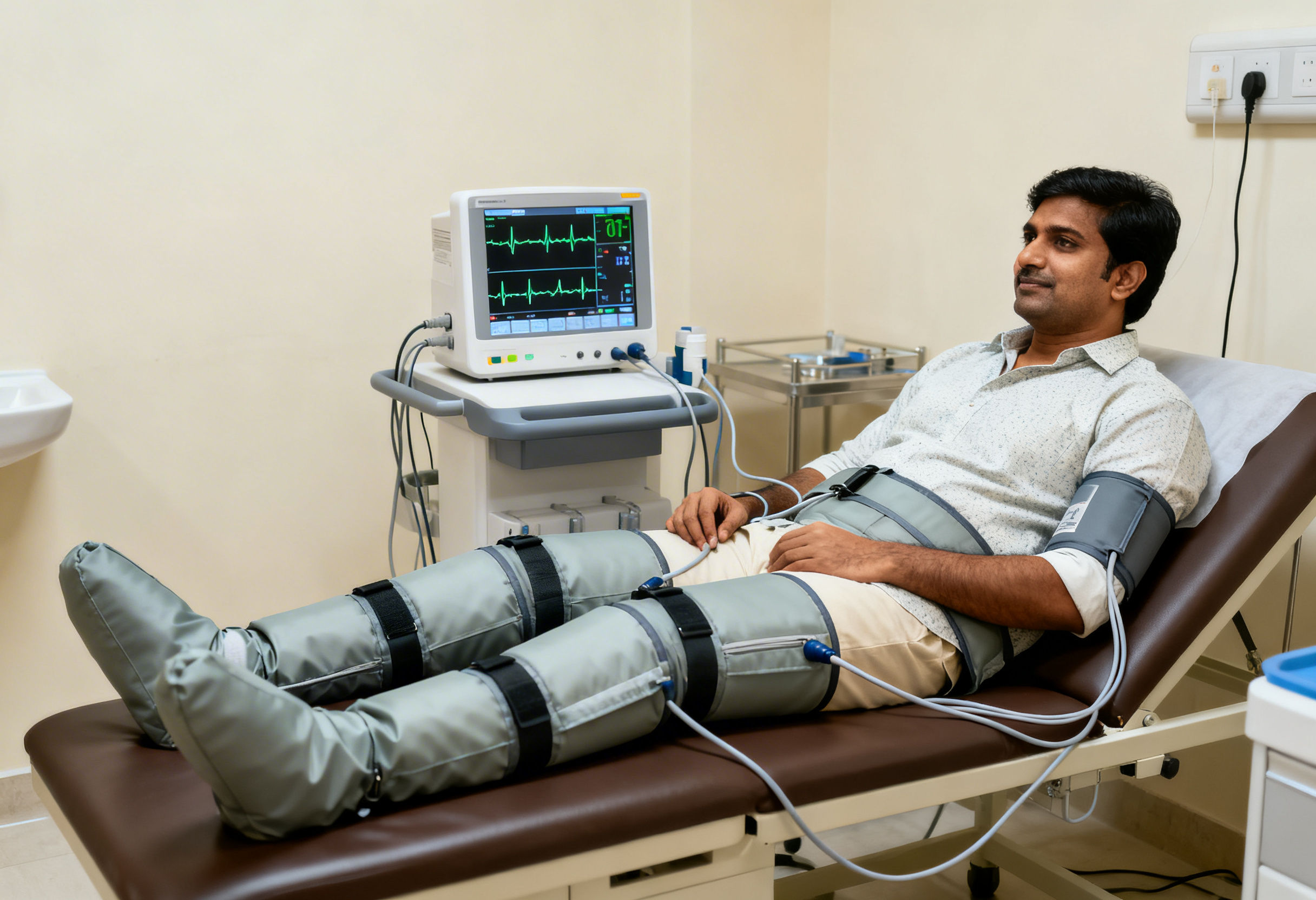
Enhanced External Counterpulsation uses pneumatic cuffs wrapped around the calves, thighs, and buttocks. These cuffs inflate and deflate in synchronization with the cardiac cycle using ECG guidance.
The mechanism is purely hemodynamic and biological.
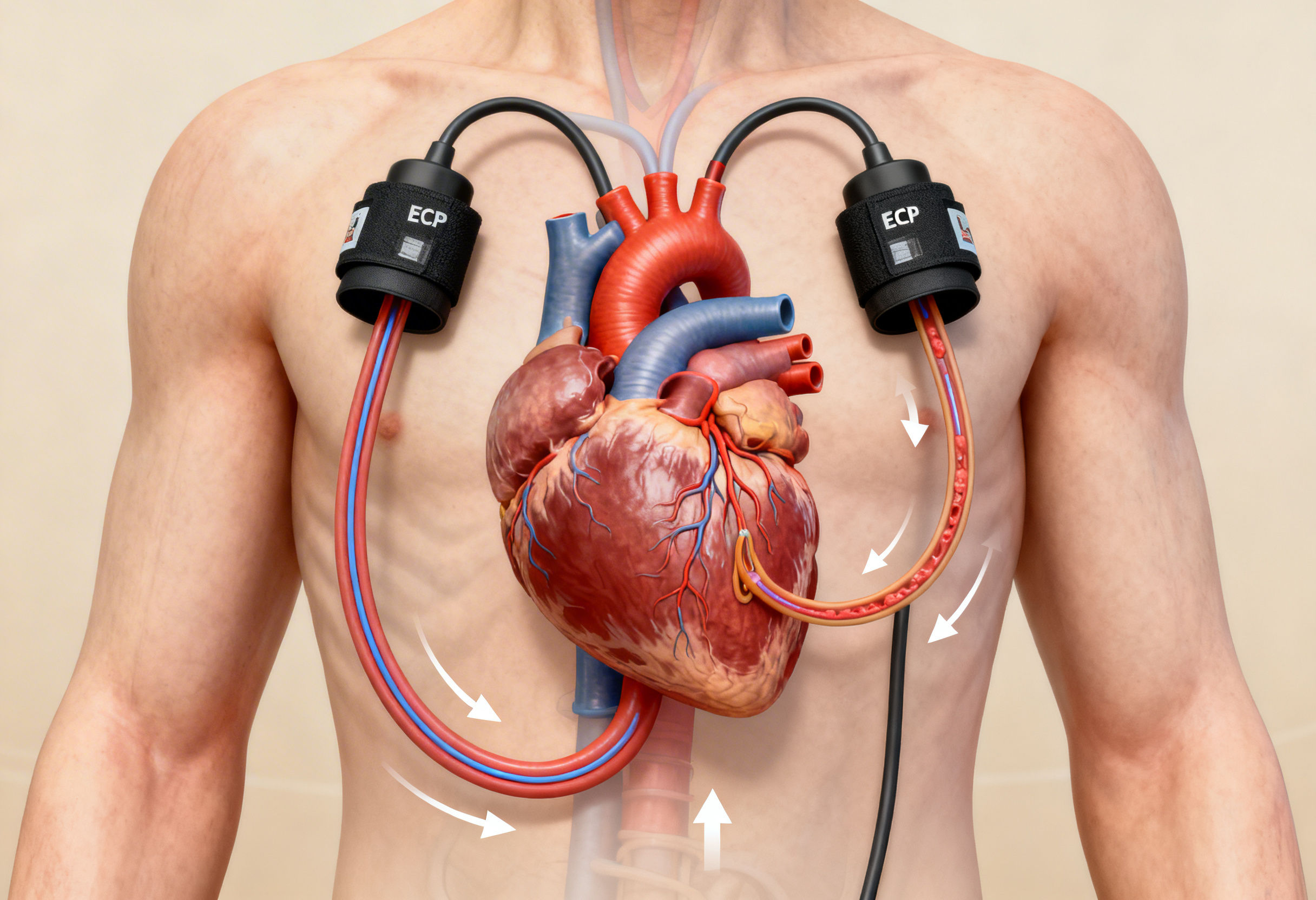
Diastolic Augmentation
During diastole, when the heart relaxes, the cuffs inflate sequentially from distal to proximal.
This generates:
- Retrograde arterial flow
• Increased aortic diastolic pressure
• Enhanced coronary perfusion
Since coronary arteries fill during diastole, this augmentation pushes oxygen rich blood into ischemic myocardium.
Systolic Unloading
Just before systole, the cuffs deflate simultaneously.
This causes:
- Reduction in systemic vascular resistance
• Decreased afterload
• Reduced myocardial oxygen demand
For diabetic patients with stiff ventricles, systolic unloading reduces cardiac strain and improves stroke volume.
Endothelial Restoration and Nitric Oxide Production
ECP therapy for diabetic heart disease also works at the cellular level.
The repeated increase in blood flow creates shear stress along endothelial surfaces. Shear stress stimulates endothelial nitric oxide synthase activity, increasing nitric oxide production.
Benefits include:
- Vasodilation
• Reduced platelet aggregation
• Anti inflammatory modulation
• Improved endothelial resilience
In diabetes, where nitric oxide production is suppressed, this restoration is clinically meaningful.
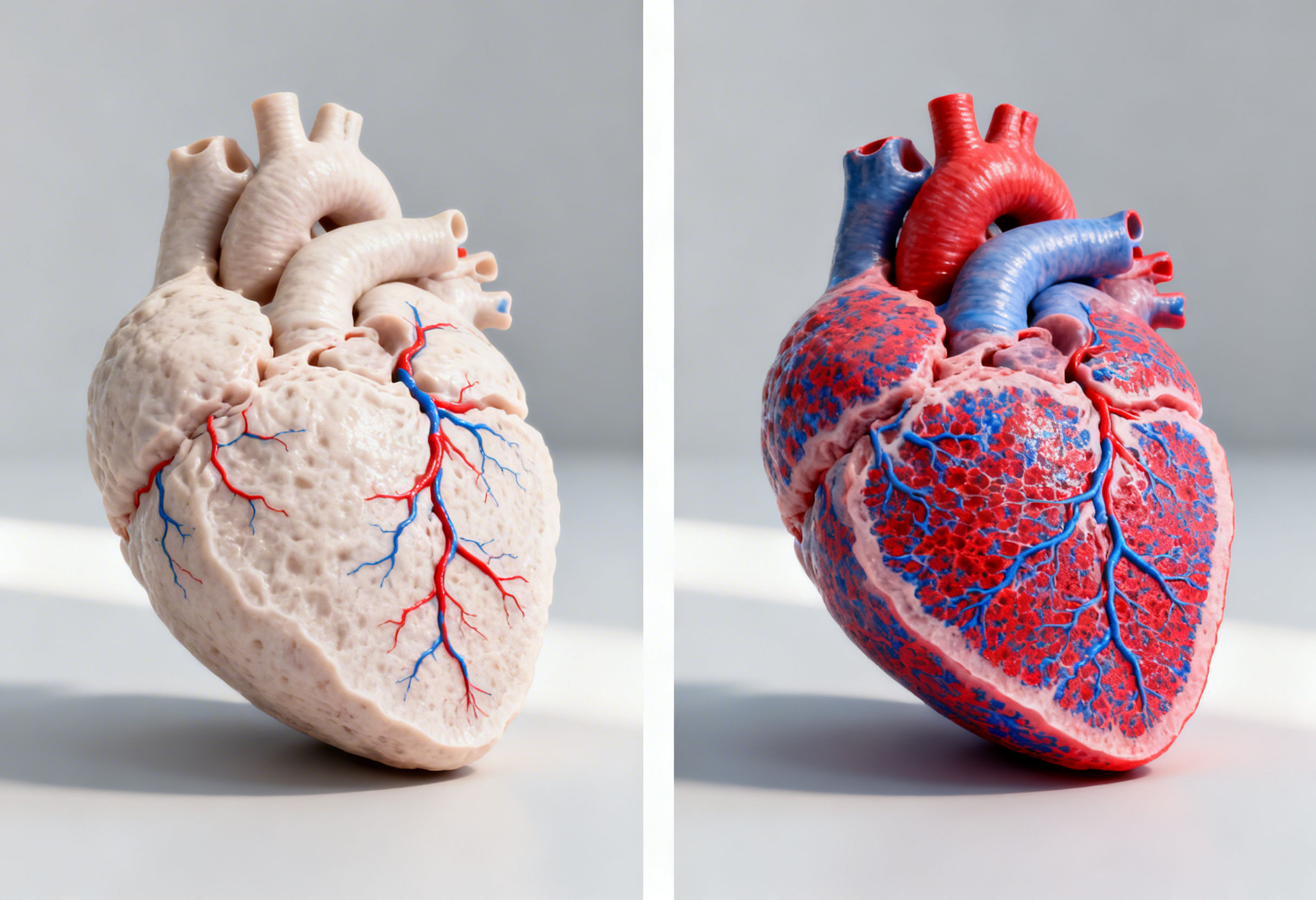
The Natural Bypass Effect
One of the most significant advantages of ECP therapy for diabetic heart disease is the stimulation of collateral circulation.
Repeated shear stress induces:
Arteriogenesis
Expansion of pre-existing collateral vessels into functional conduits capable of bypassing blocked segments.
Angiogenesis
Formation of new capillaries mediated by vascular endothelial growth factor signaling.
For patients with diffuse coronary disease not suitable for surgery, this natural bypass phenomenon improves myocardial oxygenation without invasive intervention.
Metabolic Benefits Beyond the Heart
ECP therapy behaves like an exercise mimetic in patients unable to perform vigorous physical activity.
Improved Insulin Sensitivity
The rhythmic compression stimulates skeletal muscle perfusion and enhances GLUT-4 transporter activity.
This results in:
- Better glucose uptake
• Reduced fasting glucose
• Improved insulin sensitivity index
• Reduction in HbA1c
Improved metabolic control further reduces vascular inflammation.
Reduction in Systemic Inflammation
ECP therapy lowers high sensitivity C reactive protein levels and reduces pro inflammatory cytokine activity.
Since inflammation drives both insulin resistance and endothelial dysfunction, this dual benefit is clinically significant.
Why Diabetic Heart Disease Is Frequently Missed
Autonomic neuropathy alters symptom perception.
Many patients do not experience classical angina. Instead, they report:
- Breathlessness
- General fatigue
- Exercise intolerance
Relying only on chest pain delays intervention.
Proactive vascular support using ECP therapy for diabetic heart disease may stabilize patients before acute cardiac events occur.
ECP vs Surgical Interventions in Diabetics
Diabetic patients face higher risks during invasive procedures.
Surgical Concerns
- Impaired wound healing
• Increased infection risk
• Contrast induced nephropathy
• Higher restenosis rates
• Slower recovery
Advantages of ECP
- Non invasive
• No anesthesia
• No hospital stay
• No surgical incision
• Suitable for elderly and high risk patients
ECP does not replace emergency surgery but offers an alternative for chronic stable disease management.
Treatment Protocol Overview
A standard course consists of 35 one hour sessions, typically delivered five days per week over seven weeks.
Weeks 1 to 2
Hemodynamic adaptation. Improved relaxation and mild symptom relief.
Weeks 3 to 5
Angiogenesis and endothelial activation peak. Patients often report increased stamina.
Weeks 6 to 7
Metabolic consolidation and sustained circulation improvement.
Post treatment evaluation includes stress testing and symptom reassessment.
Systems Based Care at ARKA Anugraha Hospital
At ARKA Anugraha Hospital, ECP therapy for diabetic heart disease is integrated within a multidisciplinary framework. Cardiologists collaborate with metabolic specialists to align counterpulsation therapy with glycemic optimization, nutrition guidance, and lifestyle intervention. The objective is not only symptom relief but vascular resilience and long term metabolic stabilization. Each patient undergoes structured screening to ensure safety and individualized protocol design.
Long Term Impact
Patients completing ECP therapy for diabetic heart disease frequently report:
- Reduced angina frequency
• Improved walking distance
• Better energy levels
• Stabilized blood glucose
• Reduced medication dependency in selected cases
Benefits often persist for several years when combined with sustained lifestyle changes.
FAQs
- Is ECP therapy safe for diabetic patients?
Yes. It is non-invasive and has a strong safety profile when properly screened. - Does it replace bypass surgery?
Not in emergencies. It is an alternative for chronic stable disease or high risk surgical cases. - How soon will I feel improvement?
Many patients report changes after 10 to 15 sessions. - Can it improve heart failure symptoms?
Yes, especially in patients with reduced ejection fraction. - Will it lower my HbA1c?
It can improve insulin sensitivity and contribute to better glycemic control. - Is there downtime after each session?
No. Patients can resume routine activities immediately. - Does insurance cover it?
Coverage depends on diagnosis and policy terms. - Can it help microvascular disease?
Yes. It improves capillary perfusion and collateral formation. - Is it painful?
Patients feel rhythmic pressure, not pain. - Can elderly patients undergo ECP therapy?
Yes, after proper cardiovascular assessment. - What are contraindications?
Active deep vein thrombosis, severe valvular disease, uncontrolled arrhythmias. - How long do benefits last?
Often three to five years when supported by lifestyle modification. - Can it be repeated?
Yes, booster sessions may be considered if symptoms recur. - Does it interact with medications?
No direct interaction, but medication adjustments may be required. - Is it suitable after stents?
Yes, especially if symptoms persist.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
