Prolotherapy for Back Pain: Treating the Hidden Instability Behind Chronic Suffering

- Published on: 30/Jan/2026
- Posted By: Arka Health
Priya had been living with chronic lower back pain for six years. Her story was frustratingly familiar. The pain started after lifting her toddler awkwardly from a car seat, and what began as a minor strain never truly resolved. She tried everything her doctors recommended: physiotherapy, muscle relaxants, multiple courses of pain medication, and three separate epidural steroid injections. Each intervention provided temporary relief at best, sometimes lasting just days before the deep, nagging ache returned.
Her MRI reports repeatedly came back showing “mild degenerative disc disease” and “small disc bulge at L4-L5.” Multiple specialists assured her these findings were normal for her age and could not fully explain her level of disability. Yet she could barely make it through a workday without needing to lie down. Standing to cook dinner became an ordeal. The pain radiated into her buttocks and down the back of her thigh, leading to a diagnosis of sciatica that never quite fit because the pain never extended below her knee.
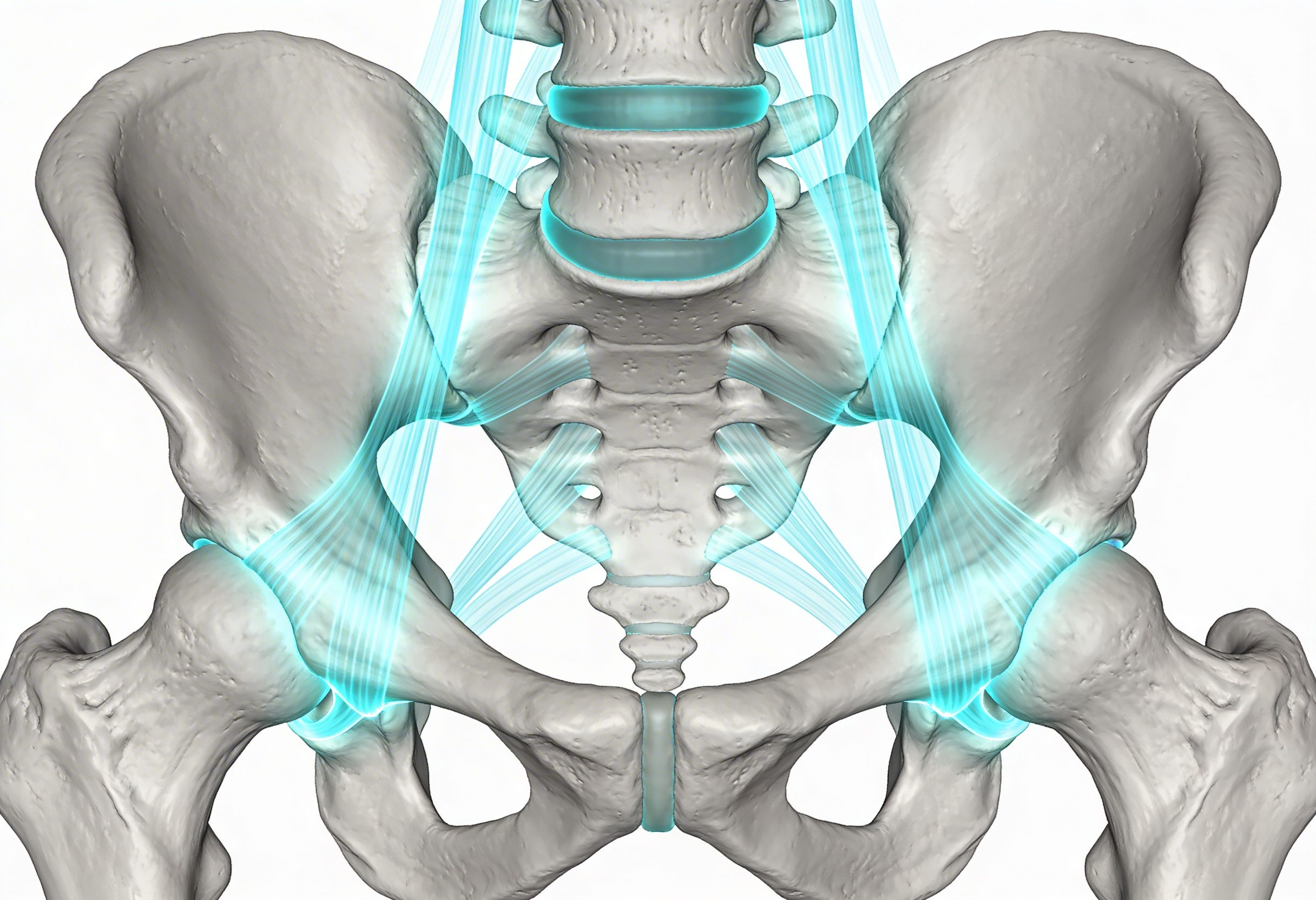
What every doctor had missed was not visible on any MRI taken while she lay perfectly still. The real problem was not her disc. It was the ligaments holding her spine together. These tough fibrous bands had become stretched and loose, creating instability that only revealed itself during movement, standing, and weight bearing. Her spine was shifting excessively with every step she took, grinding on nerves and overworking muscles desperately trying to stabilize segments that should have been held firmly by healthy ligaments.
This is the hidden reality of most chronic back pain. While medicine has focused obsessively on discs and bones, the true culprit often lies in the silent failure of the ligamentous support system. At ARKA Anugraha Hospital, we recognize this gap and address it through prolotherapy, a regenerative treatment that strengthens weakened spinal ligaments and restores the stability your spine needs to function without pain.

Understanding the Real Architecture of Spinal Stability
Your spine is not a rigid tower of stacked bones. It functions more like a sophisticated suspension bridge where bones serve as compression elements and ligaments serve as tension cables. When those cables become loose or damaged, the entire structure becomes unstable regardless of how strong the bones are.
Each segment of your spine, called a functional spinal unit, consists of two vertebrae with a disc between them, held together by a complex network of ligaments. These include the anterior and posterior longitudinal ligaments running the length of your spine, the ligamentum flavum connecting the vertebral arches, the facet joint capsules surrounding the small joints on either side, and the supraspinous and interspinous ligaments connecting the bony projections you can feel along your back.
What makes ligaments so critical is that they are not just mechanical restraints. They are densely packed with specialized nerve endings called mechanoreceptors that constantly monitor joint position and movement. In a healthy spine, when you bend or twist, these sensors detect the motion and instantly signal your deep spinal stabilizing muscles, particularly the multifidus, to contract and protect the segment. This split second ligament to muscle communication keeps your spine safe during movement.
But ligaments have a fatal weakness: they have very poor blood supply compared to muscles. When a ligament gets stretched beyond its elastic limit, whether from a sudden injury or years of poor posture and repetitive stress, it often does not heal back to its original length. The ligament remains permanently elongated, a condition called laxity. Once this happens, the protective communication system breaks down.
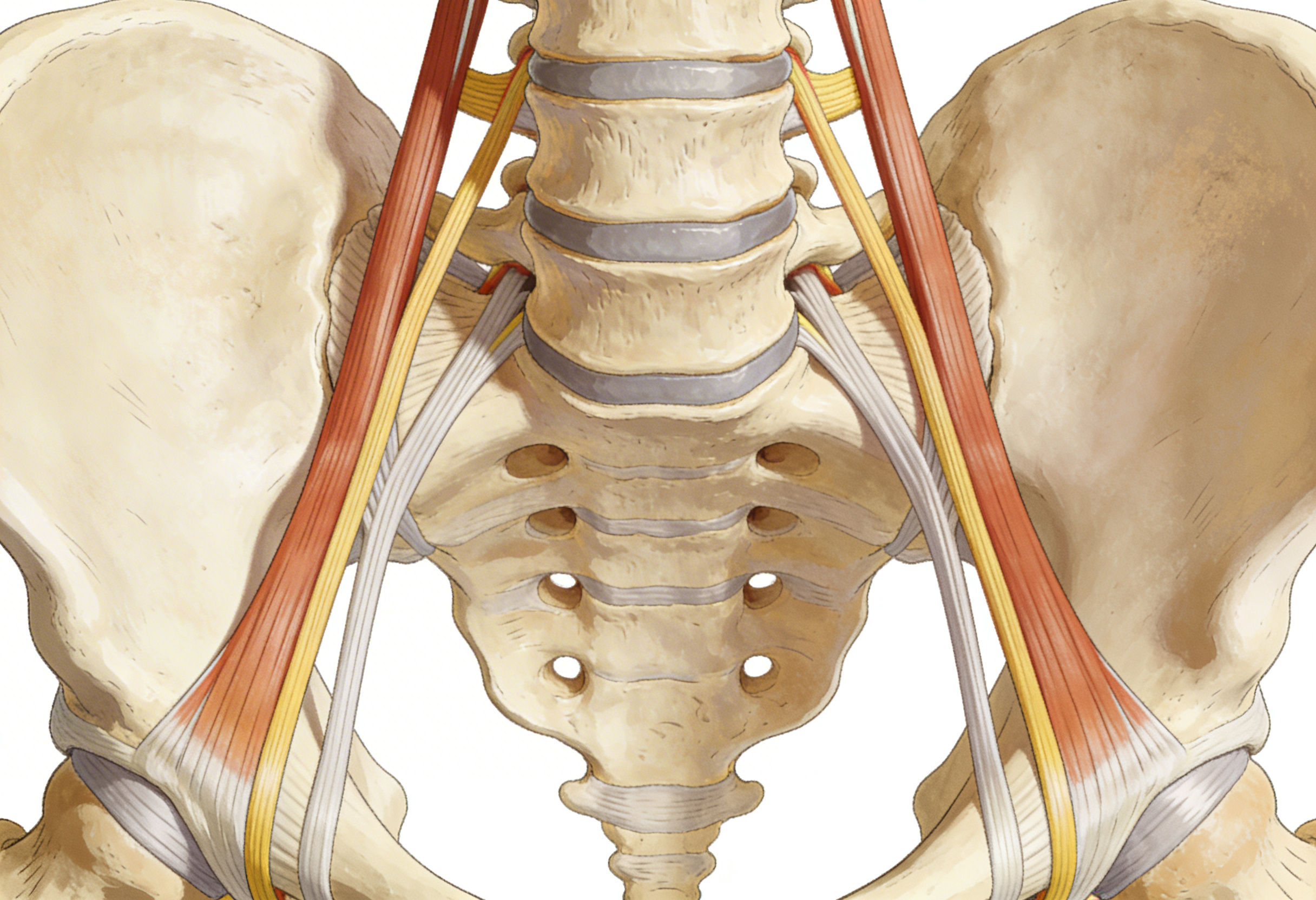
The Cascade of Damage From Spinal Instability
When spinal ligaments become lax, a predictable chain of problems unfolds. Understanding this cascade explains why your back pain persists despite normal or near normal imaging.
The loose ligaments allow excessive movement between vertebrae. This might be forward or backward sliding called translation, excessive rotation, or gapping of the facet joints. You might feel this as your back giving way, a sense of weakness, or a need to constantly crack or manipulate your spine to feel stable.
Your nervous system responds to this instability with protective muscle spasm. The mechanoreceptors in the lax ligament send alarm signals to your brain indicating the joint is not secure. Your brain responds by commanding the paraspinal muscles to contract continuously, essentially asking them to do the stabilizing job the ligaments can no longer perform. This is why you develop chronic muscle tightness and spasms that massage, stretching, and muscle relaxants cannot resolve. The tight muscles are not the problem. They are your body’s desperate compensation for loose ligaments.
This abnormal movement creates destructive forces. When vertebrae slide or rotate excessively, they subject the disc between them to abnormal shear stresses it was never designed to handle. Over time, this mechanical overload causes the disc to degenerate, lose height, and bulge. The facet joints on either side of the spine crash into each other repeatedly, accelerating arthritis. Conventional medicine then treats the degenerated disc or arthritic facets while completely ignoring the ligament laxity that caused the problem in the first place.
Finally, the shifting bones compress nerves. This produces radiating pain, numbness, and tingling that gets diagnosed as sciatica or radiculopathy. But in many cases, the nerve compression is not from the disc bulge that shows on MRI. It is from the dynamic instability allowing bones to shift and pinch nerves during certain movements or positions.
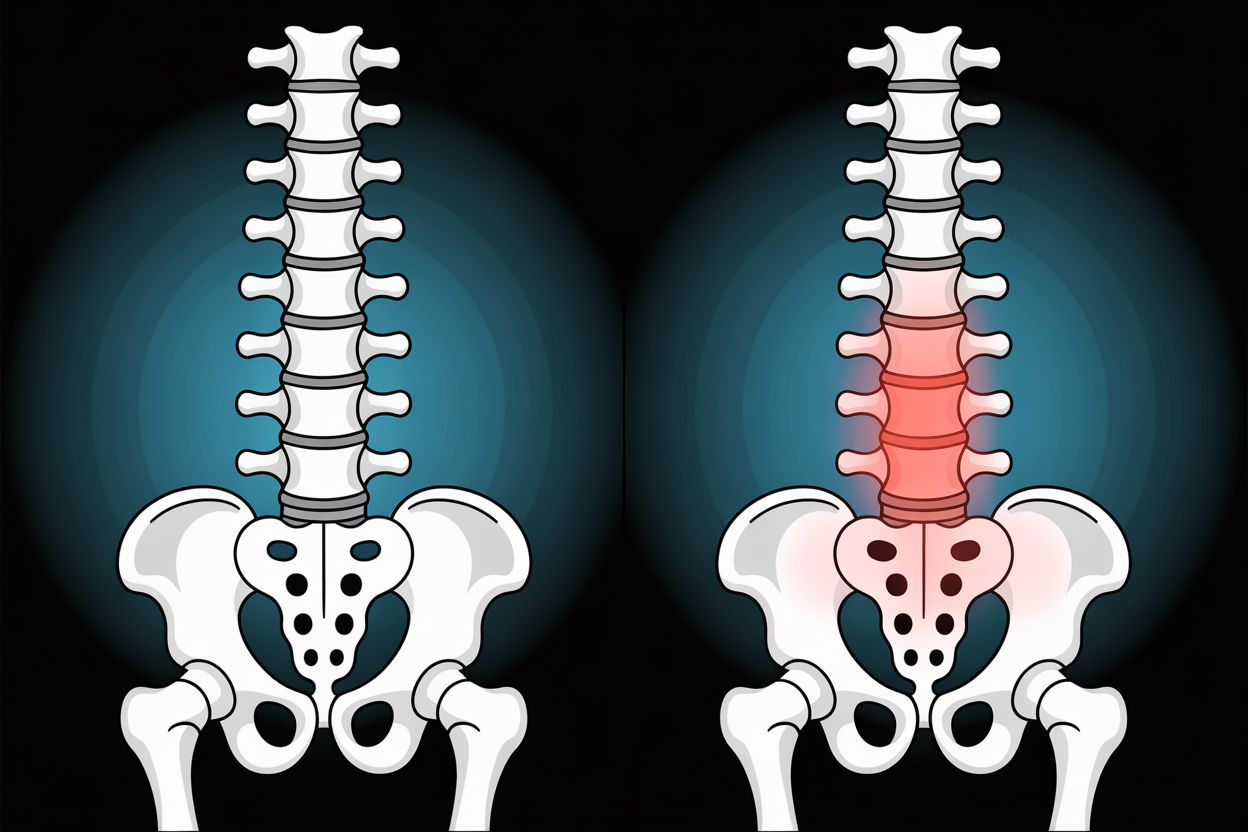
The Ligamentous Concept: Why Your Disc Is Not the Villain
For decades, medicine has operated under a disc centric model. If your back hurts and your MRI shows a disc bulge or herniation, the disc must be causing your pain. This led to countless discectomy surgeries removing the offending disc material. Yet outcomes remained disappointingly inconsistent, giving rise to the diagnosis of failed back surgery syndrome.
The ligamentous concept offers a completely different explanation. In this model, the disc is rarely the primary problem. Instead, it is a secondary victim of the instability created by ligament failure. The disc degenerates because the loose ligaments allow excessive motion that grinds it down over time.
This explains several confusing clinical observations. First, why do many people with terrible looking MRIs showing multiple bulging discs have no pain, while others with relatively normal MRIs suffer severely? The difference is stability. Someone with strong ligaments holding their spine steady can have disc abnormalities without symptoms. Someone with ligament laxity experiences pain from instability even when their discs look reasonable.
Second, why does removing the disc bulge through surgery often fail to resolve pain? Because if you decompress the nerve but do not address the underlying instability, the segment continues moving abnormally. The nerve gets re-irritated from motion rather than from the disc material itself. The pain returns because the root cause, ligament laxity, was never treated.
Prolotherapy targets the root cause. By strengthening the ligaments and restoring stability, it removes the excessive motion that damages discs and irritates nerves. The disc abnormality may remain visible on MRI, but it stops causing problems because the mechanical environment has been corrected.
Related service: Comprehensive spine evaluation at ARKA Anugraha Hospital uses functional assessment and palpation to identify ligament instability missed by standard imaging.
The Critical Spinal Ligaments and Where They Fail
Successful prolotherapy for back pain requires understanding which specific ligaments commonly fail and how their injury creates the patterns of pain patients experience.
The iliolumbar ligament is arguably the most important stabilizer of your lower back. This massive ligament connects the transverse processes of your L5 vertebra, and sometimes L4, directly to the crest of your pelvis. Its job is preventing L5 from sliding forward on the sacrum, the triangular bone at the base of your spine. When this ligament becomes lax, L5 becomes unstable and prone to slipping, a condition called spondylolisthesis.
What makes iliolumbar ligament injury particularly confusing is its referral pattern. Injury to this ligament commonly refers pain to your groin, inner thigh, and even genitals. Countless patients undergo evaluations for hernias, hip problems, or urological conditions when the real source is an unstable L5 vertebra. When your physician at ARKA Anugraha Hospital presses firmly on the attachment point of this ligament and reproduces your exact groin pain, the diagnosis becomes clear even though your MRI showed nothing.
The sacroiliac joint complex represents another common source of chronic back pain. The SI joints connect your spine to your pelvis and bear tremendous forces during walking, standing, and bending. These joints are held together by some of the strongest ligaments in your body, including the dorsal interosseous, sacrospinous, and sacrotuberous ligaments. Despite their strength, these ligaments can become lax from trauma like falls onto your buttocks, pregnancy related hormonal changes that soften ligaments, or repetitive stress from activities involving twisting.
When SI ligaments become loose, the joint becomes unstable and refers pain in a classic pattern: deep buttock pain, pain along the side of your thigh, and sometimes into your calf and foot. This mimics sciatica so closely that countless patients undergo treatment for herniated discs when their actual problem is SI joint instability. The key distinguishing feature is that true sciatica from disc herniation typically extends all the way to your foot, while SI joint pain rarely goes below your knee.
The supraspinous and interspinous ligaments run along the bony projections down the center of your back. These form what biomechanical specialists call the posterior tension band, preventing excessive forward bending. Whiplash injuries and chronic slouching posture stretch these ligaments, creating a characteristic pattern of central lower back pain that radiates vaguely into your buttocks. If you experience tenderness when pressing directly on the bumps along your spine, these ligaments are likely involved.
The facet joint capsules surround the small joints on either side of each spinal level. When discs lose height from degeneration, these facet joints override and telescope together, stretching their capsular ligaments. This creates facet syndrome, characterized by pain with extension and rotation. Strengthening these capsules through prolotherapy prevents the excessive overriding that leads to facet arthritis.
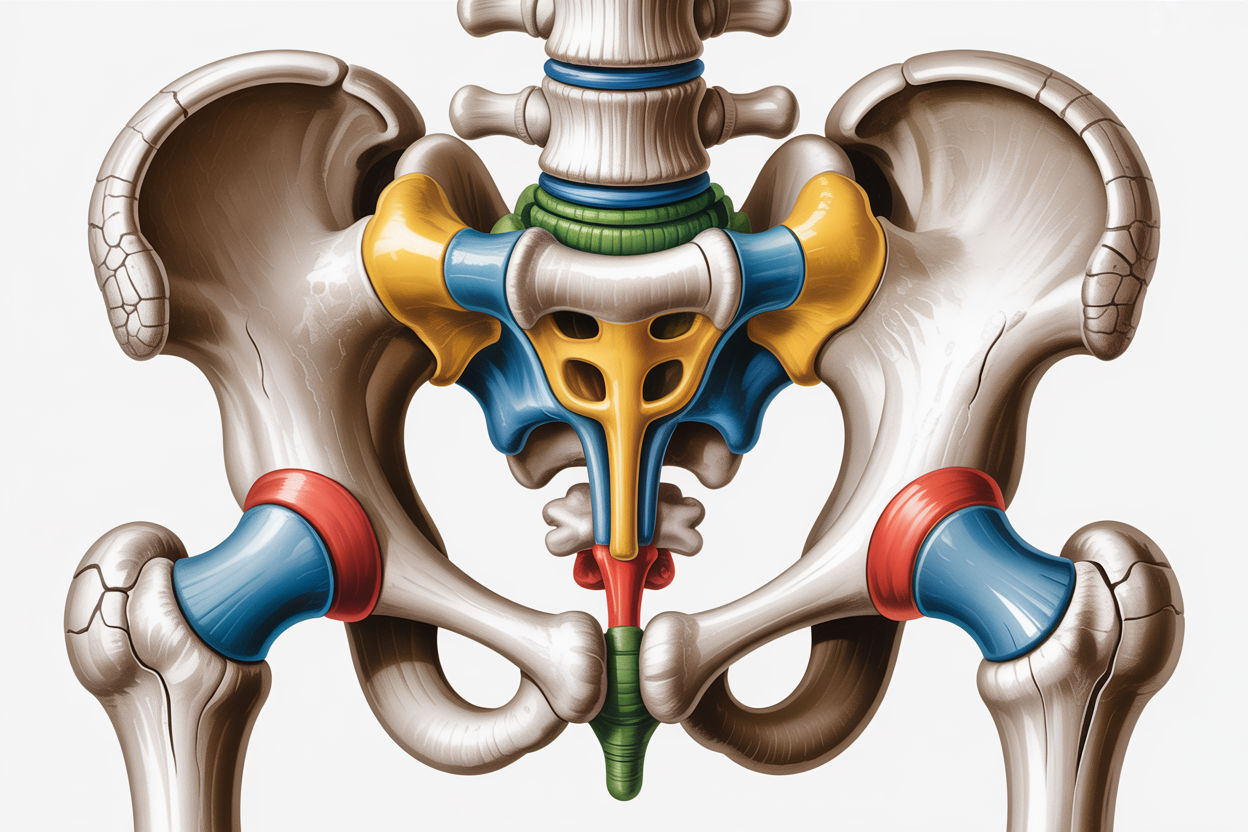
Why Standard Imaging Misses Spinal Instability
One of the most frustrating aspects of chronic back pain is being told your imaging looks normal or shows only mild changes that should not cause your level of suffering. This disconnect between imaging findings and symptom severity is not in your head. It reflects a fundamental limitation of how we image the spine.
MRI and CT scans are almost always performed with you lying flat on your back in a completely unloaded position. Gravity is not acting on your spine. Your muscles are relaxed. The vertebrae naturally settle into their most stable alignment. In this artificial position, a spine that is grossly unstable during standing, walking, or bending may look perfectly normal.
This is the static versus dynamic paradox. Ligament laxity is a dynamic functional problem that only manifests under load and during movement. A vertebra that slips excessively forward when you stand may be perfectly aligned when you lie down for your scan. The MRI captures a snapshot of your spine in its best possible position, completely missing the instability that occurs during actual function.
Additionally, ligaments themselves are difficult to visualize on standard MRI unless completely ruptured. A ligament that is intact but stretched and functionally useless looks normal on imaging. The scan shows the ligament is present but cannot assess whether it is doing its job of stabilizing the joint.
This is where advanced functional imaging becomes valuable. Digital motion X-ray, or DMX, involves taking video X-rays while you actively move through your range of motion. This dynamic imaging can reveal excessive translation where vertebrae slide too far forward or backward, gapping where facet joints open wider than they should, or asymmetrical rotation indicating one sided ligament failure. These abnormal movements explain your pain even when static MRI looked fine.
At ARKA Anugraha Hospital, we also rely heavily on palpatory examination. By pressing firmly on specific ligament attachment points while asking you to report what you feel, we can identify sensitized ligaments that reproduce your exact pain pattern. If pressing on your iliolumbar ligament recreates your groin pain, we have identified the source functionally regardless of what imaging shows.
Read next: Understanding why imaging often fails to explain chronic pain at ARKA Anugraha Hospital.
The Prolotherapy Solution for Spinal Instability
Prolotherapy for back pain works through the same fundamental mechanism described in our previous articles on general prolotherapy, but the application requires spine specific expertise and comprehensive treatment of the entire unstable segment.
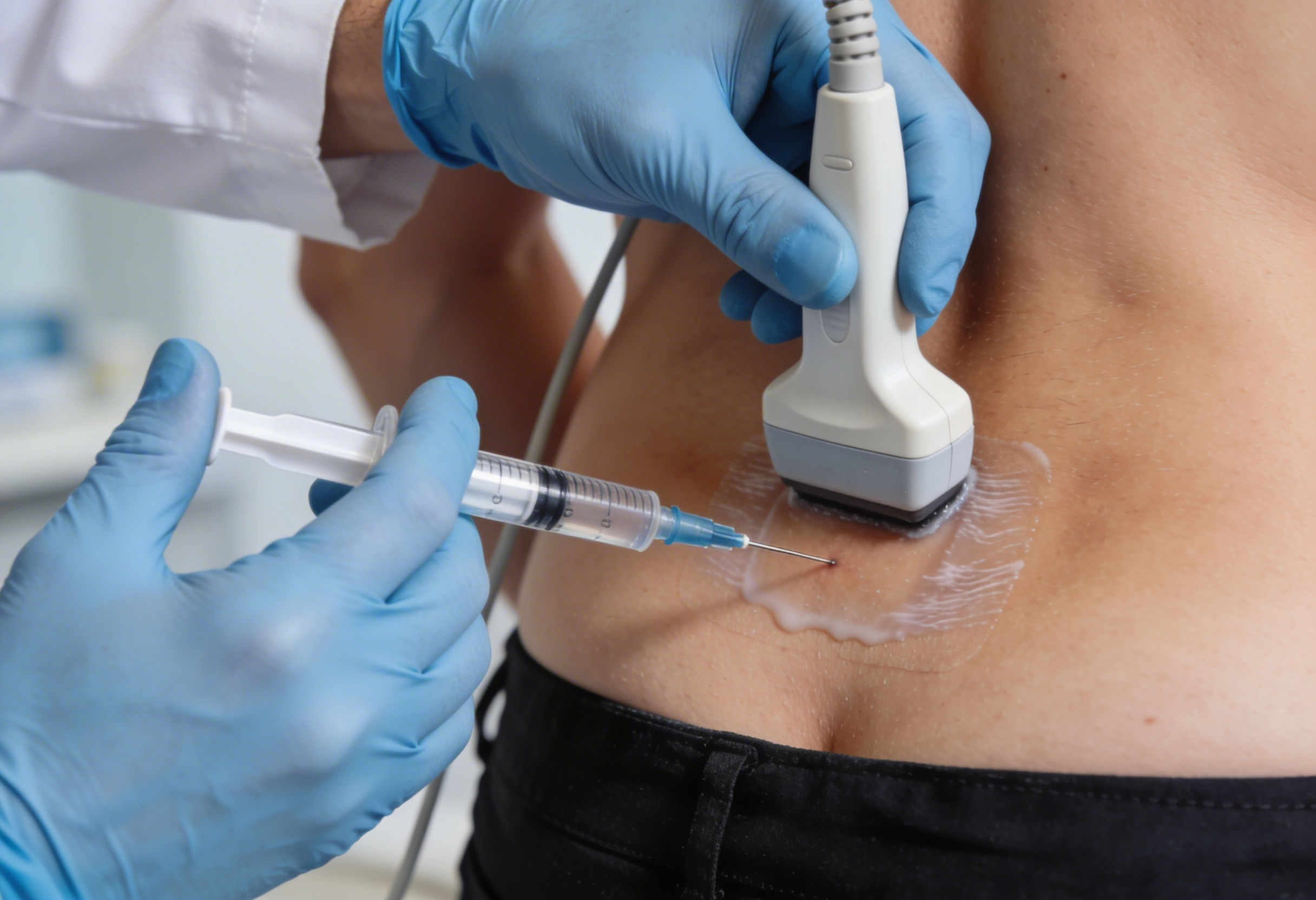
The treatment involves injecting a solution, most commonly concentrated dextrose sugar mixed with local anesthetic, directly into the weakened ligament attachments where they connect to bone. For back pain, this typically means treating the iliolumbar ligaments where they attach to L5 and the pelvis, the SI ligaments around the sacroiliac joints, the supraspinous ligaments along the spinous processes, and the facet joint capsules.
Unlike treating a single knee or elbow ligament, spinal prolotherapy often requires treating multiple levels and structures during each session. This is because the spine functions as a kinetic chain where instability at one level transfers stress to adjacent segments. A comprehensive treatment, often called the Hackett Hemwall technique, typically involves 30 to 60 milliliters of solution distributed across multiple injection points to address the entire lumbar region from L3 down through the sacrum.
The technique employed is often called peppering, where the needle is redirected through a single skin entry point to touch multiple bony attachment sites. This ensures broad coverage while minimizing the number of skin punctures, improving both effectiveness and patient comfort.
Most patients require a series of three to six treatments spaced four to six weeks apart. This interval is critical because it matches the natural biological timeline of collagen synthesis and maturation. Each treatment builds upon the strengthening achieved by the previous one, progressively tightening the ligaments and reducing abnormal motion.
The Rehabilitation Component: Activating Your Multifidus
Prolotherapy provides the signal and raw materials for ligament strengthening, but rehabilitation ensures those strengthened ligaments function optimally within your movement patterns.
The most critical muscle for spinal stability is one you have probably never heard of: the multifidus. This deep spinal muscle attaches directly to your vertebrae and facet joint capsules. Its job is providing fine motor control and segmental stability. Research consistently shows that people with chronic back pain have atrophied, dysfunctional multifidus muscles.
What happens is a vicious cycle. When your ligaments become lax and your spine unstable, your nervous system shifts reliance to the larger superficial muscles like the erector spinae. These global muscles can hold you upright but cannot provide the precise segmental control the multifidus offers. Meanwhile, the multifidus essentially shuts off and shrinks from disuse.
Reactivating this muscle is essential for long term success. At ARKA Anugraha Hospital, we teach specific isometric exercises that isolate multifidus activation without creating shear forces on healing ligaments. The classic exercise is the bird dog, where you extend opposite arm and leg while maintaining a neutral spine position. This forces your multifidus to fire to stabilize your spine against the rotational forces.
Starting rehabilitation too early or with the wrong exercises can undermine prolotherapy by stressing healing ligaments before they have gained strength. The protocol typically involves active rest for the first few days after each treatment, gentle walking and basic movements during weeks two through four, and progressive loading only after the sixth week once the remodeling phase is well underway.
One critical instruction: avoid anti inflammatory medications during treatment. NSAIDs like ibuprofen or naproxen block the very inflammatory signals that drive the healing cascade prolotherapy initiates. Taking these medications essentially neutralizes your treatment. Simple pain relievers like paracetamol are acceptable if you need them for post treatment soreness.
Prolotherapy Versus Surgery: The Biological Alternative
When conservative treatments fail and instability persists, conventional medicine typically offers spinal fusion surgery. This involves using metal rods, screws, and sometimes bone grafts to permanently lock adjacent vertebrae together, eliminating motion at that segment.
Fusion surgery can be life saving for severe cases like high grade spondylolisthesis where a vertebra has slipped dramatically forward, or for fractures and infections. However, for most cases of chronic back pain from ligament laxity, fusion represents mechanical overkill with significant downsides.
First, fusion surgery carries substantial risks including infection, nerve damage, hardware failure, and lengthy recovery requiring months before returning to normal activities. Second, eliminating motion at one spinal level inevitably increases stress on the levels above and below the fusion. This accelerated wear leads to what is called adjacent segment disease, where the neighboring discs and joints degenerate rapidly, often requiring additional surgeries years later.
Prolotherapy offers what can be thought of as biological fusion. Rather than using hardware to lock vertebrae together, it strengthens the ligaments to limit excessive motion naturally. The critical difference is that prolotherapy preserves appropriate motion while eliminating harmful instability. Your spine can still move and flex as designed, but without the excessive sliding and rotation that causes pain and degeneration.
Clinical outcomes support this approach. Studies comparing prolotherapy to epidural steroid injections for chronic back pain show that while steroids may provide better relief in the first two weeks, prolotherapy delivers vastly superior outcomes at three months, six months, and beyond. Unlike steroids which can weaken tissues with repeated use, prolotherapy creates structural improvement that continues strengthening over time.
The Whole Person Context for Spinal Healing
Successful prolotherapy depends not just on the injection technique but on your body’s capacity to execute the healing cascade once triggered. This is where the integrative approach at ARKA Anugraha Hospital becomes essential, though we have covered these principles in detail in previous articles.
Hormonal status particularly affects spinal ligaments in women. The hormone relaxin, designed to soften ligaments during pregnancy, has receptors throughout the spine. Fluctuations during menstrual cycles or persistently elevated levels can create windows of increased laxity that undermine healing. Blood sugar control matters because chronic hyperglycemia interferes with collagen synthesis and stem cell function. Gut health influences systemic inflammation that can keep fibroblasts in a defensive rather than regenerative state.
These factors are assessed and optimized before beginning prolotherapy to ensure your internal environment supports robust healing rather than weak, inadequate tissue repair.
Making Your Decision About Prolotherapy for Back Pain
If you have been struggling with chronic back pain that has not responded adequately to conventional treatments, if your MRI shows relatively normal findings despite significant symptoms, or if you have been told you need fusion surgery but want to explore less invasive options first, prolotherapy deserves serious consideration.
The ideal candidate has pain driven by ligament laxity and segmental instability rather than severe structural problems requiring surgical correction. You need reasonable overall health and the commitment to undergo a series of treatments and follow rehabilitation protocols. You must be willing to avoid anti-inflammatory medications during treatment and modify activities during the healing phases.
What prolotherapy cannot do is regenerate a severely degenerated disc or realign a spine with advanced scoliosis. For grade three or four spondylolisthesis where vertebrae have slipped dramatically, surgery may remain necessary. However, for the vast majority of chronic back pain sufferers whose real problem is ligament laxity creating instability, prolotherapy addresses the root cause that conventional medicine overlooks.
For patients like Priya, whose story opened this article, prolotherapy finally provided the solution that years of conventional treatment could not. After completing a series of five treatments over six months, combined with multifidus rehabilitation, her ligaments regained their strength and her spine its stability. The chronic pain that had defined her life for six years resolved. She returned not just to work but to playing with her children on the floor, an activity she thought she had lost forever.
Your chronic back pain does not have to be permanent. When the problem is instability rather than irreversible structural damage, when the ligaments that hold your spine together have become too loose to do their job, prolotherapy offers a path to genuine structural repair and lasting relief.
FREQUENTLY ASKED QUESTIONS
- Why does my MRI look normal when I have severe chronic back pain?
MRI scans are taken while you lie flat in an unloaded position where your spine naturally settles into its best alignment. Ligament laxity is a dynamic problem that only appears during movement, standing, and weight bearing. The excessive vertebral sliding or rotation causing your pain happens when you move, not when you lie still for imaging. Additionally, stretched ligaments look structurally intact on MRI even though they are functionally useless.
- How is back pain from ligament instability different from disc herniation pain?
Disc herniation pain typically follows specific nerve pathways down your leg in dermatomal patterns and may cause numbness or weakness. Ligament instability causes more diffuse, aching pain that shifts between sides and worsens with standing or walking. You may feel your back giving way or need to frequently crack your spine. Pain from instability often improves with lying down, while disc pain may worsen with certain positions.
- Why do I need multiple prolotherapy treatments for my back instead of just one?
Your spine has multiple levels and numerous ligaments working together as a system. Comprehensive spinal stabilization requires treating the iliolumbar ligaments, SI joint ligaments, supraspinous ligaments, and facet capsules across several vertebral levels. Each treatment builds upon previous collagen deposition, progressively tightening ligaments. The series of three to six treatments matches the biological timeline of tissue maturation and strengthening.
- Can prolotherapy help if I already have degenerative disc disease or arthritis?
Yes, often significantly. While prolotherapy cannot regenerate severely degenerated discs, much back pain from arthritis actually comes from the ligament laxity and instability rather than the structural changes themselves. By stabilizing your spine and eliminating excessive motion, prolotherapy reduces the grinding forces on arthritic joints and often dramatically improves pain even when X-rays show advanced degeneration.
- What is the multifidus muscle and why is it important for my treatment success?
The multifidus is a deep spinal muscle that attaches directly to your vertebrae and provides segmental stability. People with chronic back pain typically have atrophied, dysfunctional multifidus muscles. As prolotherapy strengthens your ligaments, specific exercises reactivate this critical stabilizer so your spine functions optimally. Without multifidus rehabilitation, even tightened ligaments may not provide full stability.
- How does prolotherapy for back pain differ from getting epidural steroid injections?
Epidural steroids suppress inflammation to temporarily reduce nerve irritation and pain, but they do not address the underlying instability causing the problem. Steroids can actually weaken tissues with repeated use. Prolotherapy stimulates ligament strengthening to restore spinal stability, addressing the root cause. Studies show prolotherapy provides superior long term outcomes even though steroids may work faster initially.
- Why might prolotherapy succeed when back surgery failed to help my pain?
Failed back surgery syndrome often occurs because the surgery addressed secondary problems like disc bulges without treating the primary cause of ligament instability. Removing disc material or fusing a segment does not strengthen loose ligaments in adjacent areas. If instability persists, pain continues or moves to other levels. Prolotherapy finally addresses the ligament laxity that was causing problems all along.
- Can prolotherapy prevent me from needing spinal fusion surgery in the future?
For many patients, yes. Prolotherapy strengthens ligaments to provide what is essentially biological fusion, limiting excessive motion without hardware. This preserves normal spinal biomechanics while eliminating harmful instability. By stabilizing your spine now, prolotherapy can halt the progression of degeneration that would eventually require surgical fusion. However, severely advanced slippage or structural problems may still require surgery.
Explore Arka Recipes
Discover recipes that blend taste with health, crafted by our experts for your well-being.

Arka Diagnostics
Discover groundbreaking diagnostic services exclusive to India, now available at Arka Health, Bangalore
